
Affected patients typically present with symptoms of itching, lacrimation, burning, vasodilation, and chemosis (Figure 1). In severe disease, concomitant corneal complications can arise, leading to vision loss.4
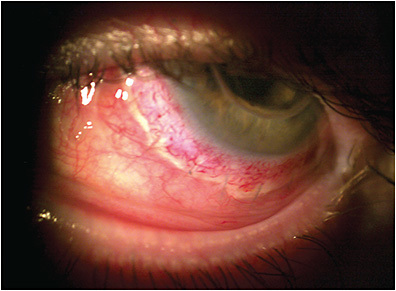
Contact lenses interact directly with the cornea, conjunctiva, tear film, and eyelids. Any homeostatic imbalance caused by ocular surface conditions, such as allergic conjunctivitis, can become exacerbated by contact lens wear leading to discomfort or lens-induced dry eye.5 As eyecare and contact lens providers, our role is to keep patients healthy and comfortable in their lenses. It is, therefore, important to understand how to detect, diagnose, and treat ocular allergy. What follows is a summary of what’s new in detection and treatment of ocular allergy.
PATIENT HISTORY AND EVALUATION
History One of the most important components of treating the allergic patient is identifying those individuals who have allergic conjunctivitis, even those who present to the office without allergic symptoms.
Many patients don’t think about reporting allergies to their eyecare providers. Interestingly, some have become so accustomed to their allergic symptoms that they don’t report them. Once we have identified these patients, we can customize their treatment options, including appropriate solutions (if indicated), contact lens modalities, materials, and therapeutic options.
Symptoms We often assume that itchy eyes indicate an allergy. Clinical experience has taught us that this isn’t the entire story. There are several forms of itching with which a patient can present, each of which is very specific to a particular ocular condition. Thus, it is critical for the examiner to be very specific when asking the patient to demonstrate the “ocular itching” that they are describing to help narrow down the diagnosis.
A patient complaining about ocular itching can present with a variety of itching habits. For example, someone who has itching of their eyelids is likely to have dermatitis.6 Someone who has itching along their eyelid margins likely has blepharitis.7 An individual who pulls their lower lid down due to itching in their lower fornix probably suffers from mucus fishing syndrome.8
An itching sensation in the inner canthal region of the eyes is often associated with seasonal allergic conjunctivitis. Patients who have this condition often experience the most itching in this area as the natural blink mechanism moves the tear film, including allergens and histamine molecules, into the inner canthal region, intensifying the allergic response.
Another form of itch is the global itch, which causes the patient to rub the entire eye with a flat palm or a fist. This is a nonspecific form of itch that may represent any of the conditions just discussed or other conditions such as dry eye, ocular infection, corneal dystrophies, etc.
Clinical Signs Inflammation is often a clinical sign of active disease. An ocular allergy is a noninfectious inflammatory condition that is the result of the ocular response to some allergen. There are several diagnostic strategies available to identify allergic disease and the sequelae of allergic eye disease on the ocular surface. Here we will discuss several of those options.
A few hallmark signs are readily visible during the biomicroscopic examination. Conjunctival hyperemia is noted as an exacerbation of inflammation. This is often a diffuse hyperemia that is visible. It is usually observed bilaterally but can be asymmetric in its presentation. Resulting from the hyperemia is the presence of chemosis, the visible swelling of the bulbar conjunctiva. Eyelid swelling is also commonly noted. The eye’s natural defense against allergens and elevated levels of histamine is tearing, so often these patients will also be visibly tearing.9
It is critical to evert the upper eyelid and assess the superior palpebral conjunctiva of any patient suspected of having allergic eye disease. The presence of papillae on the superior tarsal plate is commonly noted in allergic patients. The presence of large—or what are commonly referred to as “giant”—papillae are common in giant papillary conjunctivitis and vernal keratoconjunctivitis (VKC).4
DIAGNOSTIC TESTING
Matrix Metalloproteinase-9 (MMP-9) Testing Matrix metalloproteinase-9 is a nonspecific inflammatory enzyme that is elevated in people who have ocular surface disease. It is not specific to any one condition and, in times of inflammation, is known to be elevated. Patients who have seasonal allergic conjunctivitis have demonstrated elevated tear MMP-9 levels.10 Patients who have VKC have had the strongest relationship of elevated levels of tear MMP-9.11
There is, fortunately, a point-of-care test that is currently available to measure tear MMP-9. The binary test measures whether MMP-9 levels are greater than the normal range expected on the ocular surface. For patients whose levels are greater than 40ng/mL, the test will be positive. For those whose levels are less than that level, the test will be negative. The signal strength that is produced by this test is concentration dependent.12
A grading scale looking at the intensity was recently proposed, giving the test additional utilization in somewhat clinically quantifying the levels of inflammation on the ocular surface.13 This can serve as a benchmark of starting inflammation levels along with monitoring inflammation levels throughout treatment.
Tear Osmolarity Tear osmolarity has been used for quite some time in the assessment and monitoring of osmolarity levels in patients who have dry eye disease.14 The question is whether the test is clinically useful for individuals who have allergic eye disease.
Recently, individuals who had allergic eye disease were tested at the time of diagnosis and after treatment. Treatment was limited to copious artificial tear use. Entering measurements show that individuals who had allergic eye disease had hyperosmolar tears. After being treated with artificial tears, those whose tears returned to normal osmolarity levels also had improvements in symptoms.15 Although not commonly used in allergic eye disease management, this technology may play a role in the management of this condition.
IgE Testing Immunoglobulin E (IgE) is an antibody found on the surfaces of mast cells. The antibodies are over-expressed on the surfaces of cells in patients who have allergic conjunctivitis and are critical in the type I hypersensitivity response. Allergens bind to IgE molecules on the surfaces of mast cells, causing cross-linking of the IgE on the cell surfaces, triggering mast cell degranulation and the release of histamine in the tissue and tear film.4
IgE levels are elevated in the tear film in patients who have allergic conjunctivitis.4 Verséa Ophthalmics’ tear-based testing platform, or T-POC, relies on a portable colorimetric digital reader to determine quantitative protein concentrations of IgE in the tears. The T-POC IgE Allergy Test confirms or rules out allergic conjunctivitis. The IgE test is a lateral flow immunoassay that uses monoclonal antibodies coupled with gold nanoparticles to identify the presence of immune complexes that form between the target analyte in tears and conjugated gold particles.
The more IgE that is present, the more intense the color. The digital reader uses this information to quantify the results. Levels of IgE greater than 40ng/mL are above normal. After a sample of tears is acquired, the measurement is available in less than 10 minutes.16
TOPICAL TREATMENTS
The effective treatment for allergic conjunctivitis is avoiding the allergen. Unfortunately, this isn’t realistic for many individuals. Several therapeutic agents are available as over-the-counter options to treat allergic conjunctivitis. Ketotifen 0.025% is available under several brands and is approved for twice-a-day dosing for allergic conjunctivitis. It has antihistaminic and mast cell stabilizing effects. Recently, a preservative-free formulation of ketotifen in unit dose vials has become available. Olopatadine is available in three concentrations: 0.1%, 0.2%, and 0.7%, and also has antihistaminic and mast cell stabilizing effects. The 0.1% strength is approved as b.i.d., and the 0.2% and 0.7% strengths are approved as a q.d. dosing regimen.
Alcaftadine 0.25% recently became available as an over-the-counter option. It too has antihistaminic and mast cell stabilizing effects and is approved for a q.d. dosing regimen. A topical formulation of cetirizine has also become available as a prescription option for allergic conjunctivitis. It is available as 0.024% cetirizine and is approved for a b.i.d. dosing regimen.
At times, topical corticosteroids may be utilized for more severe presentations of allergic conjunctivitis. A formulation of loteprednol 0.2% is approved to treat seasonal allergic conjunctivitis with a q.i.d. dosing regimen. There are several other topical corticosteroids that are frequently utilized to treat severe presentations of allergic conjunctivitis. Fluorometholone, loteprednol, and prednisolone are commonly utilized topical agents.
Topical corticosteroids are sometimes used for cases of giant papillary conjunctivitis. Typically, contact lens wearers are asked to temporarily stop wearing lenses while prescribed corticosteroids to reduce ocular surface inflammation. Often, they are then fit with a more frequently replaced contact lens option. Typically, if a daily disposable is available in the patient’s prescription, this is the best option.
VKC has been traditionally treated with topical corticosteroids. Recently, a topical preservative-free prescription option, cyclosporine 0.1%, was approved to treat this condition. The advantage is that topical cyclosporine can be utilized without the concern of increases in intraocular pressure and cataract formation. This is critically important, as the patients who have the condition are typically younger males.
A new class of medications, referred to as reactive aldehyde species (RASP) inhibitors, is currently being investigated. RASP inhibitors increase in times of inflammation, including allergic conjunctivitis. Inhibiting RASP provides an opportunity to reduce clinical signs and symptoms of allergic conjunctivitis through an alternate pathway instead of traditional antihistamine mechanism of action.17 Reproxalap is a RASP inhibitor that has been shown to reduce ocular itching, tearing, and redness associated with allergic conjunctivitis.17
CONTACT LENS AND DEVICE TREATMENTS
It is commonplace in the management of ocular allergy to discontinue soft contact lens wear due to the potential for allergens to lodge in the material. Attached lens antigens cause extended exposure to the ocular surface thereby worsening allergic symptoms.18
Nevertheless, many patients, especially those who have high refractive errors and irregular astigmatism, are not able to discontinue lens wear due to the visual necessity of this modality. Maintaining ocular surface health and comfort during wear, and avoiding contact lens dropout, poses a special challenge for eyecare providers. Fortunately, new innovations and techniques in contact lens technologies have emerged, making lens wear more comfortable and even therapeutic for those who have ocular allergy. What follows is a review of these new technologies.
Therapeutic Lens Wear Contact lenses can act as a physical protective barrier for the cornea against airborne antigens. Soft lenses have been shown to decrease symptoms of lacrimation in the presence of onions19 and in the presence of pollen, decreasing burning, stinging, dryness, and itchiness compared to no lens wear.20 When soft contact lenses are worn to protect against allergens, cleaning should be emphasized and extended wear avoided. Alternatively, daily disposable lenses may be prescribed.
Prescription therapeutic lenses not only protect the ocular surface from environmental allergens but can also aid in healing when ocular allergy causes corneal21 and conjunctival complications.22 Allergic conjunctival diseases capable of causing corneal injury include VKC and atopic keratoconjunctivitis (AKC).
Patients who have seasonal and perennial allergic conjunctivitis experience itchy eyes and show conjunctival hyperemia and edema, but no corneal injury. By contrast, patients who have VKC show tarsal giant papillae (Figure 2) or limbal conjunctival swelling and are often affected by corneal injuries, resulting in eye pain and vision loss.
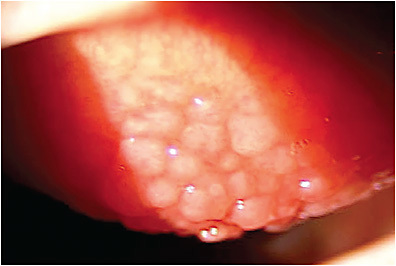
AKC is a chronic conjunctival inflammatory condition associated with palpebral and periocular allergic disease. Thickening and papillary hypertrophy of the bulbar tarsal conjunctiva are characteristic. Severe and chronic conjunctival inflammation in VKC and AKC may result in corneal lesions such as punctate keratitis, corneal erosions, corneal plaque, or corneal vascularization.4 Dry eye disease may develop in severe cases due to changes in the function and number of goblet cells and corneal nerves.23
Scleral lenses vault over the cornea. The presence of fluid underneath scleral lenses promotes healing and protects the cornea in various surface disorders such as dry eye disease, Stevens-Johnson syndrome, graft-versus-host disease, chemical injuries, and ocular allergy such as VKC.21 Moreover, the GP optics in scleral lenses correct resultant irregular astigmatism from such surface diseases.21 Additionally, patients who have severe allergic conjunctival diseases may experience cicatricial fornix changes. Scleral lenses can be used as a symblepharon ring, reducing existing advancing symblepharon, or be fitted after surgical excision to reduce recurrence.22
Soft hydrogel lenses can also be used to heal corneal complications such as vernal ulcers (Figure 3).24 Soft lenses can be used in conjunction with dehydrated amniotic membrane transplantation (AMT) to help heal corneal injuries (Figure 4)25 such as persistent epithelial defects from complications in shield ulcers from VKC.26 Cryopreserved amniotic membrane can also be placed using soft contact lenses in an alternate “sandwich technique.”27 This involves taking a soft lens and using a hole punch device to remove the center optic, creating a soft skirt ring.

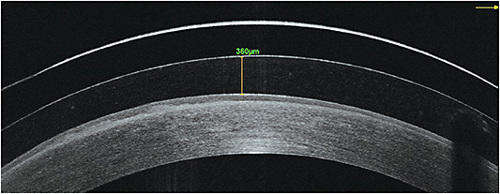
Next, the skirt ring is placed on the ocular surface in the same fashion as would an unaltered soft lens. After this, the cryopreserved amniotic membrane is cut in the same shape and diameter as the central ring opening of the soft lens. This cut amniotic membrane is then placed into the center opening of the soft lens ring. Last, an unaltered soft lens is piggybacked on top to hold it all in place.27
Interestingly, the authors have had experience with patients who are habitual scleral contact lens wearers and needed AMT for healing corneal defects. Both dehydrated and cryopreserved membranes have been placed in the bowls of scleral lenses successfully, aiding in healing corneal complications. Similarly, topical medications such as artificial tears, autologous serum, and anti-VEGF medications can be placed in the bowl of a scleral lens (Figure 4) to help heal corneal defects caused by severe ocular allergy such as punctate keratitis28 and corneal neovascularization.29
Drug-Eluting Lens Devices Topical formulations are a common treatment for ocular allergy and other anterior segment diseases, and they account for more than 90% of ophthalmic medications.30 Topical medications are rapidly removed by the nasolacrimal duct and restoration of tear film and are also eliminated by conjunctival blood and lymphatic flow.31 Thus, only 1% to 5% of the administered topical medication is absorbed into the tissue.32 To counter this problem of low bioavailability, frequent instillation of topical medications is usually needed, which can impact patient compliance.
Instead of topical medications, drug-eluting contact lenses may be an alternative method of treatment for eye conditions. Since drug delivery via therapeutic lenses increases the time of the medication in front of the cornea, its bioavailability may increase to approximately 50%, enhancing drug efficacy and minimizing side effects.33 The contact lens platform may also encourage patient treatment compliance due to the elimination of multiple administrations of drops throughout the day, especially in those wearing lenses for visual correction.
With respect to treatment of ocular allergy, drug-eluting soft lenses with medications such as mast cell stabilizers and antihistamine combinations34 and corticosteroids35 have been developed. In fact, a ketotifen-eluting daily disposable soft contact lens was approved by the U.S. Food and Drug Administration in 2022 for ocular allergy. The effectiveness of this contact lens delivery system is comparable to that of direct topical drug delivery of ketotifen alone.34
SUMMARY
Allergic conjunctivitis is common and may be experienced by anyone who has a history of allergies. Avoiding allergens is difficult, if not impossible, so treatment for allergies focuses on managing symptoms and limiting detrimental side effects of the inflammatory disease process. There are a variety of diagnostic signs and supportive tests that can confirm the presence of allergic conjunctivitis and grade its severity. Treatments include topical pharmaceuticals as well as contact lenses, including some that elute drugs. Regardless, the goal of treatment is to stabilize and protect the ocular surface, thereby preserving eye health and vision. CLS
References
- Burbach GJ, Heinzerling LM, Rohnelt C, et al. Ragweed sensitization in Europe - GA(2)LEN study suggests increasing prevalence. Allergy. 2009 Apr;64:664-665.
- Guarnieri M, Balmes JR. Outdoor air pollution and asthma. Lancet. 2014 May;383:1581-1592.
- Abelson MB, Smith L, Chapin M. Ocular allergic disease: mechanisms, disease sub-types, treatment. Ocul Surf. 2003 Jul;1:127-149.
- Villegas BV, Benitez-del-Castillo JM. Current Knowledge in Allergic Conjunctivitis. Turk J Ophthalmol. 2021 Jan;51:45-54.
- Nichols JJ, Willcox MDP, Bron AJ, et al. The TFOS International Workshop on Contact Lens Discomfort: Executive Summary. Invest Ophthalmol Vis Sci. 2013 Oct;54:TFOS7-TFOS13.
- Zirwas MJ. Contact Dermatitis to Cosmetics. Clin Rev Allergy Immunol. 2019;56:119-128.
- Bernardes TF, Bonfioli AA. Blepharitis. Semin Ophthalmol. 2010 May;25:79-83.
- Chiew RLJ, Au Eong DTM, Au Eong KG. Mucus fishing syndrome. BMJ Case Rep. 2022 Apr;15:e249188.
- Bielory L, Delgado L, Katelaris CH, Leonard A, Rosario N, Vichyanoud P. ICON: Diagnosis and management of allergic conjunctivitis. Ann Allergy Asthma Immunol. 2020 Feb;124:118-134.
- Acera A, Rocha G, Vecino E, Lema I, Duran JA. Inflammatory markers in the tears of patients with ocular surface disease. Ophthalmic Res. 2008 Oct;40:315-321.
- Leonardi A, Sathe S, Bortolotti M, Beaton A, Sack R. Cytokines, matrix metalloproteases, angiogenic and growth factors in tears of normal subjects and vernal keratoconjunctivitis patients. Allergy.2009 Apr;64:710-717.
- Sambursky R. Presence or absence of ocular surface inflammation directs clinical and therapeutic management of dry eye. Clin Ophthalmol. 2016 Sep;10:2337-2343.
- Brujic M, Kading D. Making Matrix Metalloproteinase-9 Levels More Meaningful. Poster presented at the 2016 Global Specialty Lens Symposium, Las Vegas. January 2016.
- Versura P, Campos EC. TearLab(R) Osmolarity System for diagnosing dry eye. Expert Rev Mol Diagn. 2013 Mar;13:119-129.
- Nitoda E, Lavaris A, Laios K, et al. Tear Film Osmolarity in Subjects with Acute Allergic Rhinoconjunctivitis. In Vivo. 2018 Mar-Apr;32:403-408.
- Ophthalmics, V., T-POC IgE Test Package Insert.
- Clark, D, Karpecki P, Salapatek AM, Sheppard JD, Brady TC. Reproxalap Improves Signs and Symptoms of Allergic Conjunctivitis in an Allergen Chamber: A Real-World Model of Allergen Exposure. Clin Ophthalmol. 2022 Jan;16:15-23.
- Lemp MA, Bielory L. Contact Lenses and Associated Anterior Segment Disorders: Dry Eye Disease, Blepharitis, and Allergy. Immunol Allergy Clin North Am. 2008 Feb;28:105-117, vi-vii.
- Higashihara H, Yokoi N, Mruyama K, et al. Effect of Lachrymatory Factor from Onion on Human Tear Secretion. Investig Ophthalmol Vis Sci. 2004 May;45:3896-3896.
- Wolffsohn JS, Emberlin JC. Role of contact lenses in relieving ocular allergy. Cont Lens Anterior Eye. 2011 Aug;34:169-172.
- Rathi VM, Mandathara PS, Vaddavilla PK, Dumpati S, Chakrabarti T, Sangwan VS. Fluid-filled scleral contact lenses in vernal keratoconjunctivitis. Eye Contact Lens. 2012 May;38:203-206.
- Campbell R, Caroline P. RGP Scleral Lenses for Stevens-Johnson Syndrome. Contact Lens Spectrum. 1997 May;12. Available at clspectrum.com/issues/1997/may-1997/rgp-scleral-lenses-for-stevens-johnson-syndrome . Accessed March 15, 2023.
- Villani E, Strologo MD, Pichi F, et al., Dry Eye in Vernal Keratoconjunctivitis: A Cross-Sectional Comparative Study. Medicine. 2015 Oct;94:e1648.
- Quah SA, Hemmerdinger C, Nicholson S, Kaye SB. Treatment of Refractory Vernal Ulcers With Large-Diameter Bandage Contact Lenses. Eye Contact Lens. 2006 Sep;32:245-247.
- Hauswirth SG. Beyond the Basics: Tackling Amniotic Membrane Therapy Complications. Rev Optom. 2017 Jan;154:42-46.
- Sridhar MS, Sangwan VS, Bansal AK, Rao GN. Amniotic membrane transplantation in the management of shield ulcers of vernal keratoconjunctivitis. Ophthalmol. 2001 Jul;108:1218-1222.
- Luccarelli SV, Villani E, Lucentini S, et al. Sutureless “Contact Lens Sandwich” Technique for Amniotic Membrane Therapy of Central Corneal Ulcers. Eur J Ophthalmol. 2022 Jul;32:2141-2147.
- Semeraro F, Forbice E, Braga O, Bova A, Salvatore AD, Azzolini C. Evaluation of the efficacy of 50% autologous serum eye drops in different ocular surface pathologies. Biomed Res Int. Epub 2014 July.
- Yin J, Jacobs DS. Long-term outcome of using Prosthetic Replacement of Ocular Surface Ecosystem (PROSE) as a drug delivery system for bevacizumab in the treatment of corneal neovascularization. Ocul Surf. 2019 Jan;17:134-141.
- Lang JC. Ocular drug delivery conventional ocular formulations. Adv Drug Deliv Rev. 1995 Aug;16:39-43.
- Janagam DR, Wu L, Lowe TL. Nanoparticles for drug delivery to the anterior segment of the eye. Adv Drug Deliv Rev. 2017 Dec;122:31-64.
- Novack GD. Ophthalmic drug delivery: development and regulatory considerations. Clin Pharmacol Ther. 2009 Feb;85:539-543.
- Bengani L, Chauhan A. Are contact lenses the solution for effective ophthalmic drug delivery? Future Med Chem. 2012 Nov;4:2141-2143.
- Ono J, Toshida H. Use of Ketotifen Fumarate-Eluting Daily Disposable Soft Contact Lens in Management of Ocular Allergy: Literature Review and Report of Two Cases. Cureus. 2022 Jul;14:e27093.
- Bengani LC, Kobashi H, Ross AE, et al. Steroid-eluting contact lenses for corneal and intraocular inflammation. Acta Biomater. 2020 Oct;116:149-161.




