SILICONE HYDROGEL (SiHy) materials were commercialized 25 years ago and now account for almost 80% of all new lenses fitted internationally. This article will discuss the pros and cons of SiHy contact lenses for refractive indications, including the effects on complications of wear. It also will review how these characteristics inform contemporary specialty contact lens practice, discuss new indications for wear, and offer suggestions for how to optimize wearer outcomes.
SiHy and the International Contact Lens Market
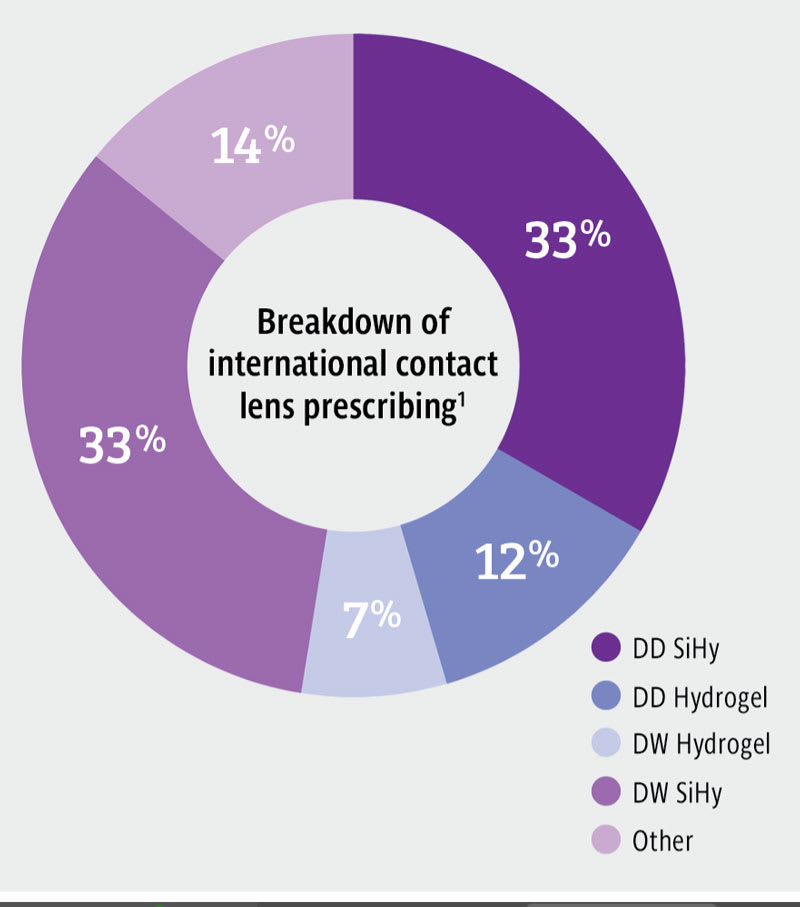
Based on the 2023 report on international contact lens prescribing, SiHys are 3 times more commonly prescribed internationally than hydrogel materials for new fittings, daily disposable lenses are more commonly prescribed than other replacement options, and extended wear is infrequently prescribed on average1 (Figure 1). It is worth noting however, that there is considerable variation between regions and countries.
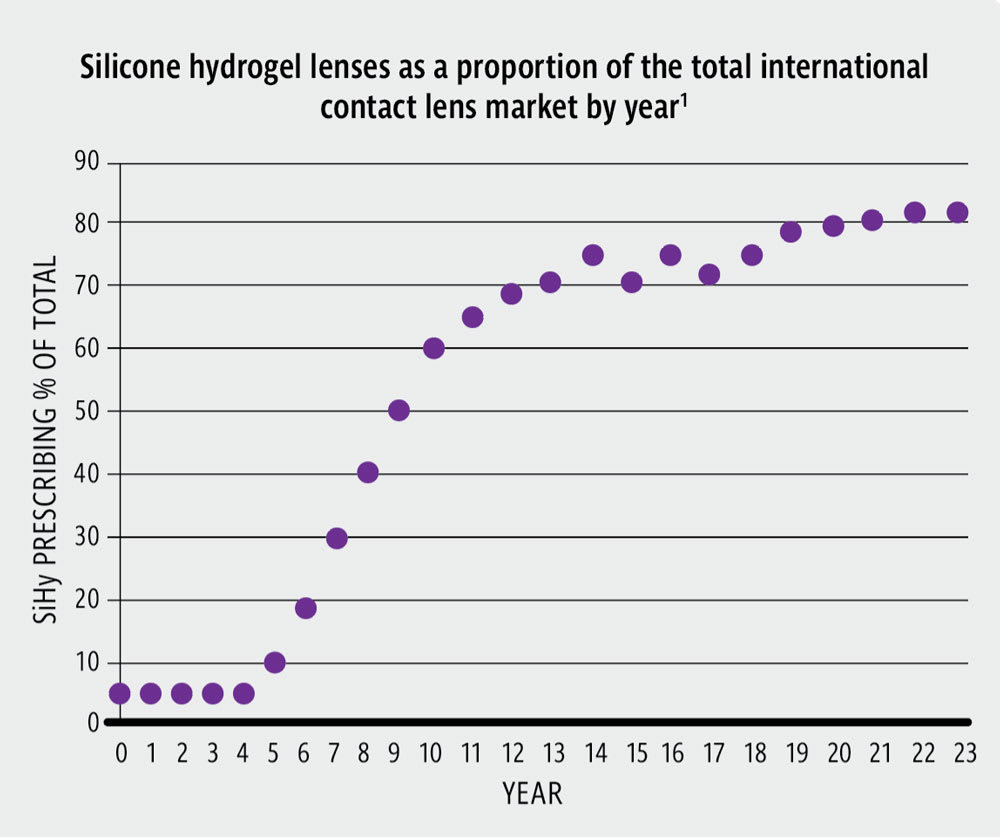
In a further analysis, the proportion of SiHys as a total of the market over time was presented, showing a slow start for 5 years and increasing to 80% of new fittings by 2020 (Figure 2).
Asia has emerged as a major and increasing market for contact lenses, accounting for 74% of worldwide sales in 2020 (euromonitor.com), which has been attributed to increased urbanization, awareness of the increase in myopia rates, and the impact of myopia. Historically, there has been low penetration of SiHy lenses, conceivably due to cost.
Colored or cosmetic lenses are a large part of the market, and approximately 75% of them are made of hydrogel materials. Licensing of contact lenses varies across Asia, and alternative (non-practitioner) supply routes are common, which makes estimating numbers of wearers in the region or lens sales data more difficult to interpret.
Pros and Cons of Managing Refractive Errors
Due to the current high penetration of SiHy materials, the metabolic sequelae2 and complications3 of contact lenses are largely consigned to history. The impact of high refractive errors4 and long-term wear is likely to be modulated by an individual’s oxygen demand.
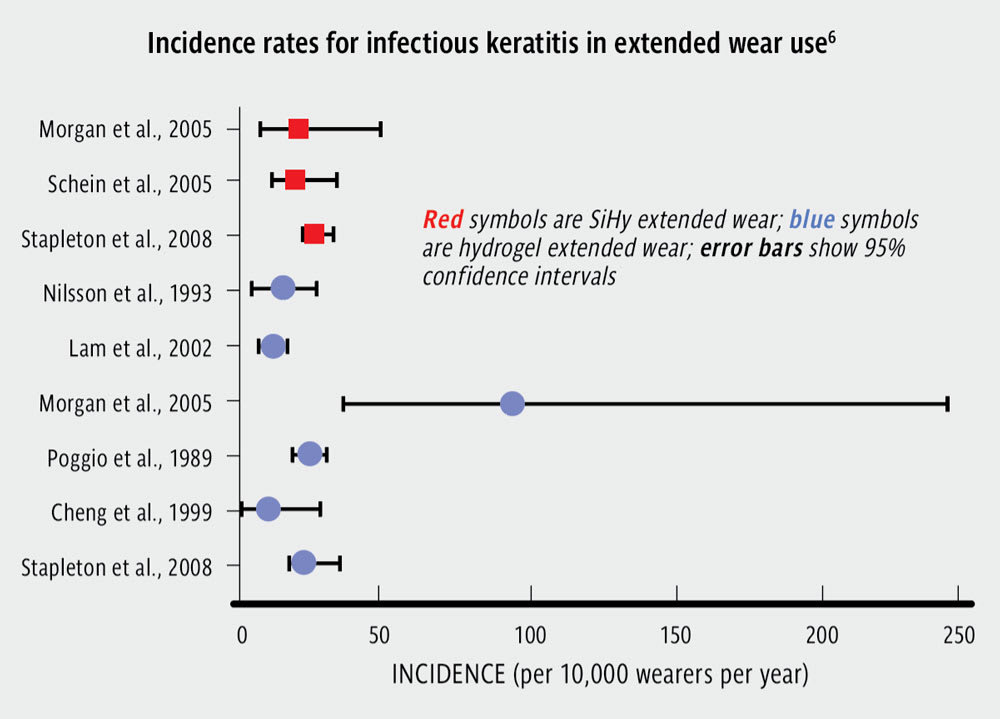
There is limited evidence of the incidence rate of infectious keratitis beyond that of early-generation lenses, but we see similar incidence rates in wearers of extended-wear SiHy and hydrogel lenses—1 in 400 per year5,6 (Figure 3). Material type appears to have no impact in 2 more recent case control studies,7,8 and SiHy lens wearers have a microbial profile9 and rate of vision loss5 from infectious keratitis similar to those of hydrogel contact lens wearers. A recent Cochrane review has concluded that there is no evidence that specific materials affect the rate of vision-threatening disease.10 There is limited evidence that the materials in cosmetic or decorative lenses cause corneal infections, noting the overrepresentation of hydrogel materials for these applications in Asia.11
The rate of infiltrates reported for both daily and extended wear of early generation SiHy lenses was twice that of hydrogel lenses.12 Daily disposable contact lenses reduce the rate of infiltrates to that of reusable contact lens use by 3 to 12 times, but material type has not been demonstrated to have an effect in multivariable analysis.13
Observation Information
While SiHy materials are increasingly used for specialty lenses, high-level evidence of their superiority is generally unavailable, although case reports are frequently published.
• Pediatric contact lens practice SiHy lens use has been frequently reported in pediatric aphakia, including recommendations for expected lens parameters.14 Historically, SiHy was limited for these applications due to the lack of parameter range, although there is much less restriction currently. The cost of loss or frequent replacement may persist as a barrier,15 particularly in some markets.
In myopia control contact lens use in children, there is no high-level evidence to suggest that there is a difference in safety between daily disposable hydrogel and SiHy contact lenses designed for myopia control and multifocal contact lenses.16,17 Theoretically, a higher Dk/t may encourage recommendations for a longer wear time to lower the risk of hypoxia-related consequences and consequently better adherence to the modality, although there is no published evidence for this.
• Bandage or therapeutic contact lens use SiHy lenses may be prescribed to maintain or restore the integrity of the ocular tissues, to treat ocular discomfort, or to protect the cornea from the environment or mechanical interactions with the lids.14 These applications may be off label for certain adult or pediatric cases. Broad indications and evidence for SiHy use are described in Table 1.
While several studies indicate that SiHy lenses are safe and effective in certain situations (post-laser epithelial keratomileusis [LASEK], pain relief, epithelial healing in wounds or corneal burns, neurotrophic disease, post-corneal cross-linking [CXL]),14 there is limited evidence to support the selection of one type over another. And, as would be expected, there are very few randomized clinical trials that have directly compared modalities.18 There may, however, be unique opportunities for SiHy materials as a cellular substrate in, for example, limbal stem cell disease,19 due to their support of corneal epithelial cell outgrowth. SiHy materials may also be a vehicle for sutureless cryopreserved or dehydrated amniotic membrane placement and retention20 and in drug delivery applications.21
• Custom lens options Custom lenses, sometimes called rehabilitative lenses, can be used to improve visual function in cases of high, irregular, or asymmetric refractive error.14 SiHy custom lenses, like hydrogel contact lenses, can be produced in a range of base curve radii, diameters, and refractive powers. Designs may be multifocal, non-coaxial, quadrant specific, and may incorporate toric optics, variable base curve, or peripheral curve to control centration and allow oblate designs. Indications include nonstandard corneal shape, high refractive error and low vision applications, and irregular astigmatism and keratoconus.24
Piggyback modalities may be indicated in normal eyes, eyes that have corneal ectasia and in which tolerance to rigid corneal lens use has reduced, or eyes that have a bleb formation or excessive apical corneal staining. Approaches may include custom or standard SiHy lenses. A daily disposable modality is recommended to limit the requirements to care for 2 different contact lens types. Highly oxygen-permeable materials have been recommended for both rigid corneal and soft contact lens components.25
Optimizing Outcomes
Although these issues are not specific to SiHy lens use, it is relevant to consider comorbidities including allergy, dry eye, meibomian gland dysfunction, anterior blepharitis, blinking abnormalities, anatomical variations, and Demodexinfestation. In pediatric applications, there may also be altered immune status and lifestyle and behavioral differences compared with adults, particularly considering the patients’ interaction with the digital world. For diseased eyes, it is useful to consider the natural history of the underlying condition and understanding and communicating the primary reason for lens fitting, risk benefit considerations, and complications.26
Written or digital patient information can include the expected wear schedule, handling, care of lenses, duration of indication, wearer consent, and follow-up schedule,26 plus instructions on the use of concomitant medications.
Summary
The altered material chemistry of SiHy lenses has changed the profile of complications seen in the wear of lenses for the correction of low refractive errors, particularly in reducing hypoxia-related complications and potential benefits of long-term wear. For severe complications, the rate and profile of infectious keratitis appear unaltered by material type. And, while certain inflammatory complications may be higher with early-generation high-oxygen-permeable materials when used on a reusable basis, these differences are not apparent in daily disposable modalities.
Clearly, SiHy specialty lenses offer an expanded scope of indications, including those for pediatric populations, newer refractive and therapeutic procedures, and diseased eyes. As material developments progress, options for disease detection and treatment are likely to increase.
References
1. Morgan PB, et al. International contact lens prescribing in 2023. Contact Lens Spectrum. 2024;39:20-28. clspectrum.com/issues/2024/januaryfebruary/international-contact-lens-prescribing-in-2023
2. Morgan PB, Murphy PJ, Gifford KL, et al. BCLA CLEAR – Effect of contact lens materials and designs on the anatomy and physiology of the eye. Cont Lens Anterior Eye. 2021;44(2):192-219. doi: 10.1016/j.clae.2021.02.006
3. Stapleton F, Bakkar M, Carnt N, et al. BCLA CLEAR – Contact lens complications. Cont Lens Anterior Eye. 2021;44(2):330-367. doi: 10.1016/j.clae.2024.102190
4. Moezzi AM, Fonn D, Varikooty J, Simpson TL. Overnight corneal swelling with high and low powered silicone hydrogel lenses. J Optom. 2015;8(1):19-26. doi: 10.1016/j.optom.2014.03.002
5. Stapleton F, Keay L, Edwards K, et al. The incidence of contact lens-related microbial keratitis in Australia. Ophthalmology. 2008;115(10):1655-1662. doi: 10.1016/j.ophtha.2008.04.002
6. Szczotka-Flynn LB, Shovlin JP, Schnider CM, et al. American Academy of Optometry Microbial Keratitis Think Tank. Optom Vision Sci. 2021;98(3):182-198. doi: 10.1097/OPX.0000000000001664
7. Szczotka-Flynn LB, Raghupathy S, Shah S, Suri K, Briggs F, Iyengar SK. Risk factors for bacterial keratitis and severe disease in hydrogel contact lens users: a multicenter case-control study and case-only analysis. Eye Contact Lens. 2024;50(11):461-466. doi: 10.1097/ICL.0000000000001125
8. Lim CH, Carnt NA, Farook M, et al. Risk factors for contact lens-related microbial keratitis in Singapore. Eye (Lond). 2016;30(3):447-455. doi: 10.1038/eye.2015.250
9. Stapleton F. Contact lens-related corneal infection in Australia. Clin Exp Optom. 2020;103(4):408-417. doi: 10.1111/cxo.13082
10. Haworth K, Travis D, Leslie L, Fuller D, Pucker AD. Silicone hydrogel versus hydrogel soft contact lenses for differences in patient-reported eye comfort and safety. Cochrane Database Syst Rev. 2023;9(9):CD01479. doi: 10.1002/14651858.CD014791.pub2
11. Stapleton F, Lim CHL, Kweon S, Tan D, Mehta JS. Cosmetic contact lens-related corneal infections in Asia. Am J Ophthalmol. 2021;229:176-183. doi: 10.1016/j.ajo.2021.03.005
12. Chalmers RL, Keay L, McNally J, Kern J. Multicenter case-control study of the role of lens materials and care products on the development of corneal infiltrates. Optom Vis Sci. 2012;89(3):316-325. doi: 10.1097/OPX.0b013e318240c7ff
13. Chalmers RL, Hickson-Curran SB, Keay L, Gleason WJ, Albright R. Rates of adverse events with hydrogel and silicone hydrogel daily disposable lenses in a large postmarket surveillance registry: the TEMPO Registry. Invest Ophthalmol Vis Sci. 2015;56(1):654-663. doi: 10.1167/iovs.14-15582
14. Jacobs DS, Carrasquillo KG, Cottrell PD, et al. BCLA CLEAR – Medical use of contact lenses. Cont Lens Anterior Eye. 2021;44(2):289-329. doi: 10.1016/j.clae.2021.02.002
15. Şengör T, Gençağa Atakan T. Management of contact lenses and visual development in pediatric aphakia. Turk J Ophthalmol. 2024;54(2):90-102. doi: 10.4274/tjo.galenos.2023.56252
16. Sankaridurg P, Bakaraju RC, Naduvilath T, et al. Myopia control with novel central and peripheral plus contact lenses and extended depth of focus contact lenses: 2 year results from a randomised clinical trial. Ophthalmic Physiol Opt. 2019;39(4):294-307. doi: 10.1111/opo.12621
17. Chamberlain P, Peixoto-de-Matos SC, Logan NS, Ngo C, Jones D, Young G. A 3-year randomized clinical trial of MiSight lenses for myopia control. Optom Vis Sci. 2019;96(8):556-567. doi: 10.1097/OPX.0000000000001410
18. Travis D, Haworth K, Leslie L, Fuller D, Pucker AD. Silicone hydrogel versus hydrogel soft contact lenses for differences in patient-reported eye comfort and safety: a Cochrane systematic review summary. Optom Vis Sci. 2024;101(9):547-555. doi: 10.1097/OPX.0000000000002161
19. Di Girolamo N, Bosch M, Zamora K, Coroneo MT, Wakefield D, Watson SL. A contact lens-based technique for expansion and transplantation of autologous epithelial progenitors for ocular surface reconstruction. Transplantation. 2009;87(10):1571-1578. doi: 10.1097/TP.0b013e3181a4bbf2
20. Travé-Huarte S, Wolffsohn JS. Sutureless dehydrated amniotic membrane (Omnigen) application using a specialised bandage contact lens (OmniLenz) for the treatment of dry eye disease: a 6-month randomised control trial. Medicina (Kaunas). 2024;60(6):985. doi: 10.3390/medicina60060985
21. Jones L, Hui A, Phan CM, et al. CLEAR – Contact lens technologies of the future. Cont Lens Anterior Eye. 2021;44(2):398-430. doi: 10.1016/j.clae.2021.02.007
22. Sun YZ, Guo L, Zhang FS. Curative effect assessment of bandage contact lens in neurogenic keratitis. Int J Ophthalmol. 2014;7(6):980-983. doi: 10.3980/j.issn.2222-3959.2014.06.12
23. Liu L, Fukuyama T, Han T, et al. Observation and assessment of the immediate use of a silicon hydrogel contact lens after transepithelial corneal cross linking: a prospective study. BMC Ophthalmol. 2023;23(1):471. doi: 10.1186/s12886-023-03217-4
24. Su S, Johns L, Rah M, Ryan R, Barr J. Clinical performance of KeraSoft® IC in irregular corneas. Clin Ophthalmol. 2015;9:1953-1964. doi: 10.2147/OPTH.S87176
25. López-Alemany A, González-Méijome JM, Almeida JB, Parafita MA, Refojo MF. Oxygen transmissibility of piggyback systems with conventional soft and silicone hydrogel contact lenses. Cornea. 2006;25(2):214-219. doi: 10.1097/01.ico.0000178276.90892.ac
26. Zhu B, Liu Y, Lin L, et al. Characteristics of infectious keratitis in bandage contact lens wear patients. Eye Contact Lens. 2019;45(6):356-359. doi: 10.1097/ICL.0000000000000593