We have settled into an academic world largely fueled by access to information on the internet. Sources for such information on myopia management include databases, online journals, private websites, blogs, reposted articles and sources, and open-source references. Information that years ago was limited can now be overwhelmingly excessive at times, requiring us to sort through data and sources to find relevant and credible information.
In light of the many myopia management tools in our toolbox, our prescribing patterns must be informed by evidence-based literature. To design myopia management treatment plans with confidence and authority, we need to refer to credible publications and studies, particularly to randomized clinical trials. In addition, when comanaging with other healthcare providers, evidence for clinical decision-making is essential to maintain trust and support.
An editorial published in 1996 stated: “Evidence-based medicine is the conscientious, explicit, and judicious use of current best evidence in making decisions about the care of individual patients.”1
In the decades since this statement was published, our understanding of best evidence-based medicine now encompasses both research and patients’ preferences. In other words, true clinical expertise balances scientific research with a patient’s clinical presentation and personal preferences. A patient or a patient’s caregiver may present a spectrum of viewpoints pertaining to the patient’s medical care depending on various factors, such as perceptions of risk versus benefit; financial or insurance considerations; personal or family lifestyle experiences; and knowledge specific to information relevant to the condition.
It has never been more important to integrate into practice the following aspects of myopia management:
- a traditional assessment for clinical findings that are outside of normative data and for risk of myopia progression;
- the need for modern myopia management, with a goal to halt or slow the progression of myopia;
- an understanding of the evidence and of the tools available to create a myopia management plan;
- patient preferences; and
- patient real-world actions
Practitioners must be prepared to address patients’ and caregivers’ questions and concerns, chief among them: Does an increasing level of myopia and controlling its progression really matter? Are the treatments safe? What treatment will work best?
In this article, we strive to give you the information that you need to answer these frequently asked questions (FAQs).
THE BASIC EVIDENCE
Myopia is one of the most common eye conditions worldwide and has become a major public health concern. The prevalence of myopia has increased rapidly over the last few decades, now reaching pandemic rates. In 2000, the World Health Organization estimated that 23% of the world’s population was myopic, with 3% having high myopia, defined as a refractive error of –5.00D or higher; with current trends, that number is projected to rise to 50% and 10%, respectively, by 2050.2 What’s more, myopia is being diagnosed at younger ages, leading to faster progression and to higher levels of the condition.3
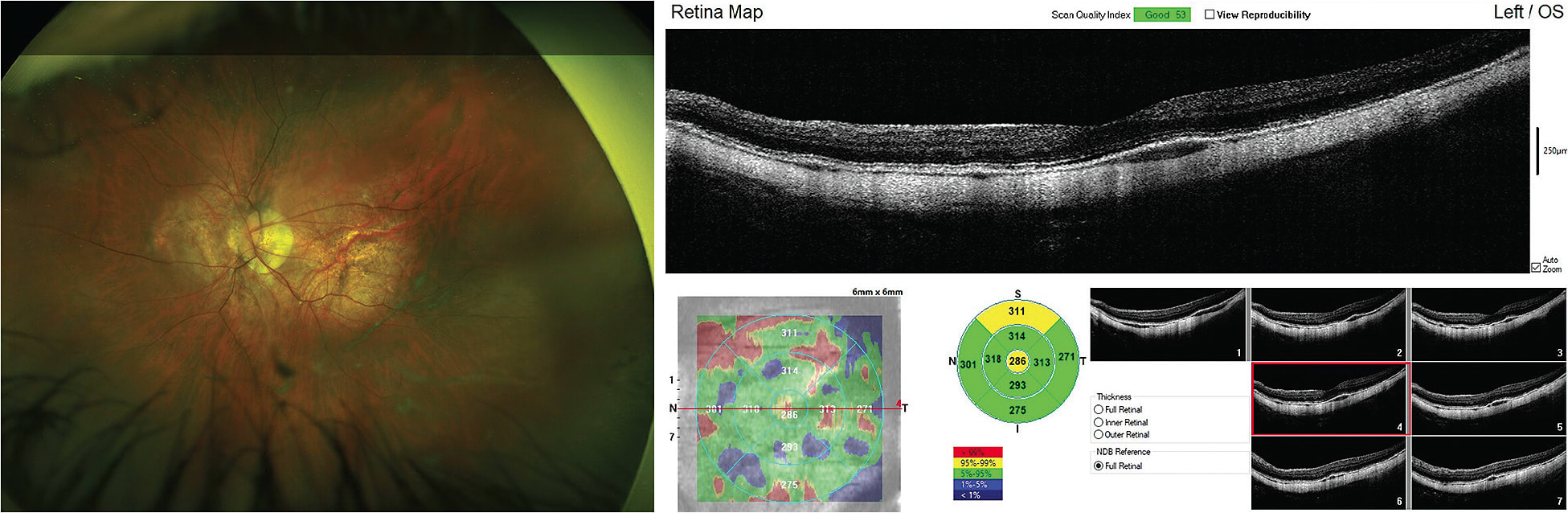
FAQ: Does an increasing level of myopia and controlling its progression really matter? Historically, myopia was perceived as a minor inconvenience that could be corrected with eyeglasses, contact lenses, or refractive surgery. Today, it is considered a significant threat to vision. As the dioptric value of myopia increases, the eye elongates and causes biomechanical stretching that may harm ocular structures.4 Excessive eye length leads to an increased risk of various degenerative conditions such as myopic maculopathy (Figure 1), which is untreatable and may cause irreversible vision loss.4 Myopia-related vision impairment may lead to reduced quality of life related to physical, emotional, and social functioning. There is also an economic burden associated with myopia.5
The cause and progression of myopia are proposed to be a multifactorial mechanism of genetic predisposition coupled with external environmental factors, particularly prolonged near work and less time spent outdoors.6 Reducing the final degree of myopia by 1.00D has the potential to reduce the likelihood of developing myopic maculopathy by about 40%.4 Hence, strategies aimed at reducing any amount of myopic refractive error have become the recommended standard of care.
Evidence-based literature has shown that optical and pharmaceutical interventions work to slow or halt myopia progression while providing good-quality vision.7 These various safe and effective interventions are paramount in providing a tailored approach to each individual patient, and they hold promise to curb the global myopia pandemic.2
ORTHOKERATOLOGY
Orthokeratology (ortho-k) is a technique whereby reverse-geometry GP contact lenses are worn overnight to reshape the cornea, resulting in temporary and reversible refractive error reduction and freedom from correction during the day. The mechanism of effect seems to occur from the reorganization of the corneal epithelium from the central cornea toward the midperiphery.8 The central corneal flattening is the treatment zone that results in the reduction in myopic refractive error, with a surrounding annulus of midperipheral steepening creating the desired bull’s-eye pattern. The greatest topographical changes occur after the first night and typically stabilize after one-to-two weeks of nightly wear.9
Ortho-k studies have demonstrated a myopia-control effect from the induced oblate corneal shape. A clear central image is focused on the fovea, with midperipheral light rays falling in front of the retina, creating a myopic defocus image shell.10 This subsequently opposes the hyperopic peripheral defocus, which is believed to be a signal for increased eye growth.10
Several studies have shown that ortho-k is an effective method to reduce axial elongation when compared to single-vision spectacle lenses.11,12 A reanalysis of these studies reported that the risk of rapid progression (axial elongation > 0.36mm/year) was reduced significantly in children wearing ortho-k lenses,13 including those who had a partial reduction of their myopia from ortho-k combined with single-vision spectacles for residual refractive error correction,14 more so with younger ages.13
Currently, the majority of studies are only two-to-three years in duration.11,12,14 One study concluded that ortho-k was effective at slowing myopia progression over a 12-year follow-up period; however, progression was monitored by spherical over-refraction changes and not by axial length.15 It is important to acknowledge that efficacy of myopia control with ortho-k can be measured only via axial elongation changes because of the need for washout to measure refraction.16 Furthermore, investigations into novel lens designs involving the manipulation of treatment zone sizes and other customizations are required to assess the potential to enhance myopia control efficacy.9
FAQ: Are ortho-k lenses safe? Safety with contact lenses is of primary concern, and ortho-k is no exception, particularly with the nature of overnight wear and the increasing number of children wearing these lenses. Nighttime wear allows parents to assist young children with lens handling and hygiene practices.9 There has been much debate over this topic; however, multiple studies and meta-analyses have shown sufficient evidence that ortho-k is safe with no long-term adverse effects.10,17,18
One of the most serious sight-threatening conditions, microbial keratitis, is generally associated with poor practice, use, or compliance with care routines (i.e., handwashing) in all types of contact lenses.10 One review estimated that the risk of microbial keratitis in ortho-k lens wearers was 13.9 per 10,000 years of wear in children and was 7.7 per 10,000 in all ages. This is comparable to the incidence of 19.5 and 25.4 per 10,000 in overnight conventional hydrogel and silicone hydrogel wearers of all ages, respectively.18
Ensuring a good lens fit is an essential aspect of contact lens safety. To further promote safety, practitioners should reinforce the importance of proper lens handling, application and removal techniques (see video below “Proper removal technique of ortho-k lens”), hygiene, and avoidance of tap water at each follow-up appointment.9
MULTIFOCAL SOFT CONTACT LENSES
Some multifocal soft lens designs have demonstrated the ability to slow myopia progression using peripheral myopic defocus. Lenses with a center-distance design have demonstrated significant reduction of myopia progression and axial elongation in several randomized controlled trials.7 The Bifocal Lenses in Nearsighted Kids (BLINK) three-year randomized clinical study suggested that +2.50D add multifocal contact lenses were more effective at slowing progression of myopia and axial length compared to +1.50D add multifocal lenses and single-vision contact lenses.19
Extended-depth-of-focus (EDOF) lenses also have been reported to slow myopia progression.20 One study evaluated a daily disposable EDOF lens design that provides clear vision through a center-distance zone, with encompassing add power up to +3.00D. This creates a blur zone at the retina that is effectively suppressed by the visual cortex and interpreted as a virtual pinhole. A drawback with this study was that it was done retrospectively and looked at the percentage of participants wearing these lenses who exhibited slowed or halted progression of myopia, a phenomenon that naturally plateaus even without interventions.20
Another daily disposable dual-focus lens became the first FDA-approved medical device indicated to slow the progression of myopia.21 In a three-year randomized, double-masked clinical trial, myopia progression and axial length were reduced in the study group compared to the control group.22 A five-year update showed good vision, safety, and efficacy, with the original control group matching the reduced refractive change and axial elongation rates of the initial treatment group after being switched to the daily disposable treatment lenses.23
After conducting a comparative study of myopia control with contact lenses in 2020, Gifford concluded:
“The comparative lifetime risks of contact lens wear commenced at age 8 for myopia control are less than the lifetime risks of vision impairment with myopia more than 6.00D or axial length more than 26mm.…Clinicians should be confident to proactively recommend myopia control contact lens wear to younger children, as both the safety profile and the potential preventative ocular health benefits are evident.”24
SPECTACLE LENSES
Commercially branded spectacle lenses, which are not yet commercially available in the United States, have been developed to reduce the relative peripheral hyperopic defocus theorized to drive the progression of myopia.25 Early investigations into undercorrection of myopia found no effect on the rate of myopia progression, or worse—possible faster progression.26 Further studies of the use of bifocals or progressive addition lenses (PALs) stemmed from the hypothesis that retinal hyperopic defocus occurs as a result of poor accommodative response and could be a factor in the development and progression of myopia. The Correction of Myopia Evaluation Trial (COMET) Study Group found a statistically significant, yet clinically insignificant, difference in myopia progression between children wearing PALs and single-vision lenses in its three-year randomized, double-masked, controlled clinical trial, and these results remained consistent after five years.27
Studies of PAL and bifocal options for myopia control have birthed a newer generation of intricate lens designs and technology at the forefront of spectacle lens options for myopia control. One defocus spectacle design consists of a central 9mm diameter correction zone with an annular zone that includes hundreds of small +3.50D add power segments in the midperiphery to simultaneously provide clear vision and peripheral myopic defocus. Results from the newly published three-year follow-up study reported a sustained myopia control effect in the children who wore defocus lenses at initiation in addition to slowed refractive and axial length changes in the control group when switched to defocus lenses after the original two-year study.28 Depending on the ages of the children, however, the natural plateau in myopia progression should not be ignored.
More recently, spectacle lenses with aspheric lenslet technology introduced the concept of a three-dimensional quantity of light in front of the retina, referred to as volume of myopic defocus. This differs from the two focal planes in the defocus spectacle lens design. The aspheric lens is made up of central distance correction surrounded by 11 concentric rings of aspheric lenslets that create the myopic defocus image shell in front of the retina. The one-year results of an ongoing randomized, double-masked, controlled clinical trial reported high refractive and axial length control efficacy when compared to single-vision lenses.29 In terms of a comparison, the defocus and aspheric lenslet designs for myopia control showed relatively similar efficacy when looking solely at the one-year results from each study.29
While the use of spectacles for myopia control was originally considered to be not as effective as contact lenses, novel myopia-control-specific spectacle lens technologies have leveled the playing field. These spectacle lenses are a viable option for patients and families who are hesitant to use contact lenses and pharmaceuticals, particularly for younger children (Figure 2). Spectacle lenses may have their place when binocular issues occur concurrently with myopia.30 Moreover, these spectacle lenses can be used in combination with full-time atropine use or alternated with daytime wear of contact lenses for slowing myopia progression; a combination of all three is useful for some patients.

LOW-DOSE ATROPINE
Atropine is a nonselective anticholinergic agent. The initial rationale behind atropine use came from the idea that its cycloplegic effects would inhibit excessive accommodation, historically believed to be responsible for myopia.31 Further research has disproved this hypothesis, and newer theories suggest that atropine interferes with the biological pathways that shape the posterior ocular structures.32 Atropine has been proposed to interrupt chemical signals for eye growth at the retina, retinal pigment epithelium, and choroid32 as well as to conserve scleral collagen structure and trigger transient increases in choroidal thickness.31
Although the exact site and mechanism driving the inhibition of eye growth in children is insufficiently understood, atropine remains an effective method to slow myopia progression, as evidenced in several clinical trials. The side effects observed with higher concentrations of atropine resulted in a shift toward lower concentrations, which have shown equivalent efficacy.33
The two-year randomized, double-masked, controlled Low-Concentration Atropine for Myopia Progression (LAMP) study revealed a concentration-dependent response for 0.05%, 0.025%, and 0.01% atropine, which resulted in 67%, 43%, and 27% reductions in refractive progression and in 51%, 29%, and 12% reductions in axial elongation, respectively. All low-dose concentrations were well tolerated.33
As younger age is associated with faster myopia progression, a recent secondary analysis suggested that younger children require a higher concentration to yield greater treatment effects. Comparable myopia progression rates were observed among 6-year-old children in the 0.05% group, 8-year-old children in the 0.025% group, and 10-year-old children in the 0.01% group.34
Low-dose atropine is regarded as a safe and effective myopia control strategy,31 particularly in patients who have high astigmatism that’s outside of the parameter ranges of the other options. Atropine may even have a role in preventing or delaying the onset of myopia; however, the idea remains inconclusive and is being studied further. Unfortunately, the anticholinergic effects of atropine can result in side effects such as mydriasis, photophobia, and loss of accommodation.31 These side effects are less common with lower concentrations and can be further mitigated by instilling the drops before sleep.
COMBINATION THERAPY
Atropine’s different mechanism of action renders it a plausible option to use in combination with other treatment methods for additive results. A review of the literature35 reported only four clinical studies on the combination of low-dose atropine and ortho-k for myopia control, all of which indicated that together the two treatments had a synergistic effect compared with ortho-k alone.
The Bifocal & Atropine in Myopia Control (BAM) Study is currently underway to investigate whether 0.01% atropine and +2.50D add center-distance multifocal soft contact lenses have a greater effect on slowing myopia progression compared to the multifocal contact lenses alone.36 It is important to acknowledge that management and complications are also additive when combining treatments; however, early results are promising and require further research. Behavior modifications such as spending time outdoors and limiting screen time still require a better evidence base to show cause-and-effect relationships, but these should be considered.
FINAL FAQ: WHAT TREATMENT WILL WORK BEST?
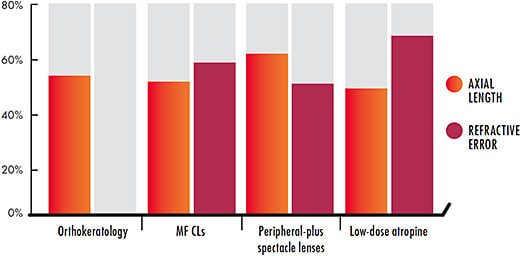
Many clinical trials have consistently demonstrated that the most effective evidence-based myopia control modalities are ortho-k contact lenses, center-distance multifocal soft contact lenses, peripheral-plus spectacle lenses, and low-dose atropine. Comparing these treatment options has proven to be difficult, given the inconsistency in the preferred metric for tracking myopia progression (refraction versus axial elongation) in addition to the wide array of study durations, participants’ ages and ethnicities, and how outcomes were expressed (dioptric values, proportions, or percentages). While each intervention has its benefits and limitations, no one method demonstrates definitive superior efficacy over the others (Figure 3).7 Efficacy is also the product of a patient’s actions and the appropriate treatment selection by a myopia management provider to best match a patient’s ocular shape, refractive error, and lifestyle.
CONCLUSION
Patient outcomes rely on our ability to source and appropriately use quality data about myopia management. Undoubtedly, I believe that the potential benefits of myopia control outweigh the risks, and collaborative evidence-based articles are particularly useful when educating and working with multidisciplinary vision and healthcare professionals. Together, through scientific discovery and communication, we can collaboratively rise. Together is better. CLS
The authors acknowledge the faculty of Pacific University College of Optometry, University of Houston College of Optometry, and University of Waterloo School of Optometry and Vision Science as well as Mission Eye Care optometrists, staff, and patients and industry partners.
REFERENCES
- Sackett DL, Rosenberg WM, Gray JA, Haynes RB, Richardson WS. Evidence based medicine: what it is and what it isn’t. BMJ. 1996 Jan;312:71-72.
- Holden BA, Fricke TR, Wilson DA, et al. Global Prevalence of Myopia and High Myopia and Temporal Trends from 2000 through 2050. Ophthalmology. 2016 May;123:1036-1042.
- Mutti DO, Hayes JR, Mitchell GL, et al. Refractive error, axial length, and relative peripheral refractive error before and after the onset of myopia. Invest Ophthalmol Vis Sci. 2007 Jun;48:2510-2519.
- Bullimore MA, Brennan NA. Myopia Control: Why Each Diopter Matters. Optom Vis Sci. 2019 Jun;96:463-465.
- Chua SYL, Foster PJ. The Economic and Societal Impact of Myopia and High Myopia. In: Ang M, Wong T, eds. Updates on Myopia, A Clinical Perspective. Singapore:Springer. 2020:53-63.
- Vagge A, Ferro Desideri L, Nucci P, Serafino M, Giannaccare G, Traverso CE. Prevention of Progression in Myopia: A Systematic Review. Diseases. 2018 Sep;6:92.
- Brennan NA, Toubouti YM, Cheng X, Bullimore MA. Efficacy in myopia control. Prog Retin Eye Res. 2021 Jul;83:100923.
- Choo JD, Caroline PJ, Harlin DD, Papas EB, Holden BA. Morphologic changes in cat epithelium following continuous wear of orthokeratology lenses: a pilot study. Cont Lens Anterior Eye. 2008 Feb;31:29-37.
- Vincent SJ, Cho P, Chan KY, et al. CLEAR – Orthokeratology. Cont Lens Anterior Eye. 2021 Apr;44:240-269.
- Cho P, Tan Q. Myopia and orthokeratology for myopia control. Clin Exp Optom. 2019 Jul;102:364-377.
- Cho P, Cheung SW. Retardation of myopia in Orthokeratology (ROMIO) study: a 2-year randomized clinical trial. Invest Ophthalmol Vis Sci. 2012 Oct;53:7077-7085.
- Chen C, Cheung SW, Cho P. Myopia control using toric orthokeratology (TO-SEE study). Invest Ophthalmol Vis Sci. 2013 Oct 3;54:6510-6517.
- Cho P, Cheung SW. Protective role of orthokeratology in reducing risk of rapid axial elongation: a reanalysis of data from the ROMIO and TO-SEE studies. Invest Ophthalmol Vis Sci. 2017 Mar;58:1411-1416.
- Charm J, Cho P. High myopia-partial reduction orthokeratology (HM-PRO): study design. Cont Lens Anterior Eye. 2013 Aug;36:164-170.
- Lee YC, Wang JH, Chiu CJ. Effect of Orthokeratology on myopia progression: twelve-year results of a retrospective cohort study. BMC Ophthalmology. 2017 Dec;17:1-8.
- Lipson MJ, Brooks MM, Koffler BH. The Role of Orthokeratology in Myopia Control: A Review. Eye Contact Lens. 2018 July;44:224-230.
- Liu YM, Xie P. The Safety of Orthokeratology—A Systematic Review. Eye Contact Lens. 2016 Jan;42:35-42.
- Bullimore MA, Sinnott LT, Jones-Jordan LA. The risk of microbial keratitis with overnight corneal reshaping lenses. Optom Vis Sci. 2013 Sep;90:937-944.
- Walline JJ, Walker MK, Mutti DO, et al. Effect of High Add Power, Medium Add Power, or Single-Vision Contact Lenses on Myopia Progression in Children: The BLINK Randomized Clinical Trial. JAMA. 2020 Aug;324:571-580.
- Cooper J, O’Connor B, Watanabe R, et al. Case Series Analysis of Myopic Progression Control With a Unique Extended Depth of Focus Multifocal Contact Lens. Eye Contact Lens. 2018 Sep;44:e16-e24.
- U.S. Food and Drug Administration. FDA approves first contact lens indicated to slow the progression of nearsightedness in children. [Press Release]. November 15, 2019. Available at https://www.fda.gov/news-events/press-announcements/fda-approves-first-contact-lens-indicated-slow-progression-nearsightedness-children . Accessed Sept. 30, 2021.
- Chamberlain P, Peixoto-de-Matos SC, Logan NS, Ngo C, Jones D, Young G. A 3-year Randomized Clinical Trial of MiSight Lenses for Myopia Control. Optom Vis Sci. 2019 Aug;96:556-567.
- Ruiz-Pomeda A, Villa-Collar C. Slowing the Progression of Myopia in Children with the MiSight Contact Lens: A Narrative Review of the Evidence. Ophthalmol Ther. 2020 Dec;9:783-795.
- Gifford KL. Childhood and lifetime risk comparison of myopia control with contact lenses. Cont Lens Anterior Eye. 2020 Feb;43:26-32.
- Li SY, Li SM, Zhou YH, et al. Effect of undercorrection on myopia progression in 12-year-old children. Graefes Arch Clin Exp Ophthalmol. 2015 Aug;253:1363-1368.
- Vasudevan B, Esposito C, Peterson C, Coronado C, Ciuffreda KJ. Under-correction of human myopia--is it myopigenic?: a retrospective analysis of clinical refraction data. J Optom. 2014 Jul-Sep;7:147-152.
- Gwiazda JE, Hyman L, Everett D, et al; The COMET Group. Five-year results from the correction of myopia evaluation trial (COMET). Invest Ophthalmol Vis Sci. 2006 May;47:1166.
- Lam CS, Tang WC, Lee PH, et al. Myopia control effect of defocus incorporated multiple segments (DIMS) spectacle lens in Chinese children: results of a 3-year follow-up study. Br J Ophthalmol. 2021 Mar 17. [Online ahead of print]
- Bao J, Yang A, Huang Y, et al. One-year myopia control efficacy of spectacle lenses with aspherical lenslets. Br J Ophthalmol. 2021 Apr 2. [Online ahead of print]
- Correction of Myopia Evaluation Trial 2 Study Group for the Pediatric Eye Disease Investigator Group. Progressive-addition lenses versus single-vision lenses for slowing progression of myopia in children with high accommodative lag and near esophoria. Invest Ophthalmol Vis Sci. 2011 Apr;52:2749-2757.
- Upadhyay A, Beuerman RW. Biological Mechanisms of Atropine Control of Myopia. Eye Contact Lens. 2020 May;46:129-135.
- Zhang Z, Zhou Y, Xie Z, et al. The effect of topical atropine on the choroidal thickness of healthy children. Sci Rep. 2016 Oct;6:34936.
- Yam JC, Jiang Y, Tang SM, et al. Low-Concentration Atropine for Myopia Progression (LAMP) Study: A Randomized, Double-Blinded, Placebo-Controlled Trial of 0.05%, 0.025%, and 0.01% Atropine Eye Drops in Myopia Control. Ophthalmology. 2019 Jan;126:113-124.
- Li FF, Zhang Y, Zhang X, et al. Age Effect on Treatment Responses to 0.05%, 0.025%, and 0.01% Atropine: Low-Concentration Atropine for Myopia Progression Study. Ophthalmology. 2021 Aug;128:1180-1187.
- Sánchez-González JM, De-Hita-Cantalejo C, Baustita-Llamas MJ, Sánchez-González MC, Capote-Puente R. The Combined Effect of Low-dose Atropine with Orthokeratology in Pediatric Myopia Control: Review of the Current Treatment Status for Myopia. J Clin Med. 2020 Jul;9:2371.
- Huang J, Mutti DO, Jones-Jordan LA, Walline JJ. Bifocal & Atropine in Myopia Study: Baseline Data and Methods. Optom Vis Sci. 2019 May;96:335-344.




