The process of treating patients with orthokeratology (ortho-k) can be a bit daunting at first. It helps to break down the process into discrete steps to understand how to make refinements. One important ortho-k tool is basic to all contact lens fitting: the over-refraction (OR).
Picking the Base Curve
It first helps to understand how the lacrimal lens works in ortho-k. The base curve (for myopia) is typically flatter than K by the amount of spherical refractive error plus an extra 0.50D to 1.00D (aka the “Jessen Factor”). The extra flatness is intended to over-treat, making the eye a bit hyperopic on lens removal. This overcomes the regression of the effect during the day so that the eyes will be closer to plano by night.
Suppose an eye has –2.00D of myopia. If we use a Jessen Factor of 0.50D, the base curve will be 2.50D flatter than K, providing –2.50D of lacrimal lens power. The ortho-k lens power is +0.50D. If measurements are accurate, you would get an over-refraction (OR) of plano.
Theoretically, as the cornea starts to flatten during treatment, the lacrimal lens will diminish in step with the corneal changes, and the OR should remain nearly plano throughout treatment.
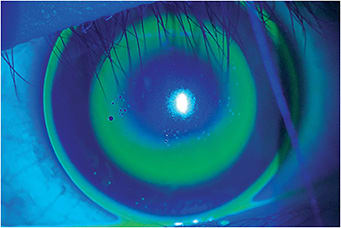
How Does the OR Help?
First, the OR is used to check that the base curve is correct at the onset of treatment. If I get an OR that is within ±0.50D, I leave the base curve alone. If I get excess plus in the OR, then there is too much minus in the lacrimal lens; this means that my base curve is too flat. If I get excess minus in the OR, the base curve is too steep; this could have happened with incorrect keratometry data or with incorrect refraction (or both).
The OR can also help troubleshoot initiated treatment. Imagine that a patient has worn the lenses for a few weeks and hasn’t hit the refractive target. If the OR is still near plano, then the problem likely is something other than the base curve (i.e., the lens sag depth is likely incorrect). If the OR is off a bit, an adjustment to the base curve (using the same steps as above) may be needed. In my experience, if you are more than 1.00D away from your refractive target, it’s probably not the base curve, and that would be reflected in the OR.
The OR can also help monitor progression of myopia. If you previously hit the refractive target, but the child is now manifesting some amount of myopia again, the refractive error may have changed or something about the lens fit could no longer be working.
If the patient refracts to –0.50D, and the OR is also –0.50D, this likely means that the fit is stable but the refraction has changed. If they don’t match up, then something about the fit is no longer optimal. Of course, it would be ideal to have axial length measurements as well to more accurately monitor progression.
In Summary
Ortho-k is a rewarding but challenging part of contact lens practice. Use the OR as one more item in your toolbox to optimize your patients’ experience with treatment. CLS