First in a series of four CE activities for 2023
LEARNING METHOD AND MEDIUM
This educational activity consists of a written article and 20 study questions. The participant should, in order, read the Activity Description listed at the beginning of this activity, read the material, answer all questions in the post test, and then complete the Activity Evaluation/Credit Request form. To receive credit for this activity, please follow the instructions provided below in the section titled To Obtain CE Credit. This educational activity should take a maximum of 2 hours to complete.
CONTENT SOURCE
This continuing education (CE) activity captures key statistics and insights from contributing faculty.
ACTIVITY DESCRIPTION
The goal of this article is to explain the use of orthokeratology as a method for both refractive correction and myopia management. Appropriate patient selection, safety and limitations to
this modality are explored, along with methods to maximize its myopia control effect.
TARGET AUDIENCE
This educational activity is intended for optometrists, contact lens specialists, and other eyecare professionals.
ACCREDITATION DESIGNATION STATEMENT
This course is COPE approved for 2 hours of CE credit.COPE Course ID: 82582-CL
DISCLOSURES
Roxanna T. Potter, OD, has taken part in non-COPE CE lectures for Contact Lens Spectrum and the GP Lens Institute.
DISCLOSURE ATTESTATION
The contributing faculty member has attested to the following:
- That the relationships/affiliations noted will not bias or otherwise influence her involvement in this activity;
- That practice recommendations given relevant to the companies with whom she has relationships/affiliations will be supported by the best available evidence or, absent evidence, will be consistent with generally accepted medical practice;
- That all reasonable clinical alternatives will be discussed when making practice recommendations.
TO OBTAIN CE CREDIT
To obtain COPE CE credit for this activity, read the material in its entirety, and consult referenced sources as necessary. We offer instant certificate processing for COPE credit. Please take the post test and evaluation online by using your OE tracker number and logging in to vccecredit.com .
Upon passing the test, you will immediately receive a printable, PDF version of your course certificate for COPE credit. On the last day of the month, all course results will be forwarded to ARBO with your OE tracker number, and your records will be updated. You must score 70% or higher to receive credit for this activity. Please make sure that you take the online post test and evaluation on a device that has printing capabilities.
NO-FEE CONTINUING EDUCATION
There are no fees for participating in and receiving credit for this CE activity.
DISCLAIMER
The views and opinions expressed in this educational activity are those of the faculty and do not necessarily represent the views of Contact Lens Spectrum. This activity is copyrighted to
Broadcastmed LLC ©2023. All rights reserved.
This activity is supported by unrestricted educational grants from AccuLens, Art Optical, and Contamac.
CE Questions? Contact CE@pentavisionmedia.com for help.
RELEASE DATE: FEBRUARY 1, 2023
EXPIRATION DATE: JANUARY 8, 2024

AS EVIDENCED BY STRIKING historical and future predictive data, the prevalence of myopia and high myopia is set to skyrocket by 2050 to levels of 49.8% and 9.8% of the world’s population, respectively.1 The rapid increase of myopia (and the ocular pathologies that increase in prevalence and severity along with higher levels) have earned this crisis the title of pandemic. As global awareness of the myopia pandemic rises, interest in methods of myopia control are intensifying as well.
Orthokeratology (ortho-k) is an overnight-wear contact lens modality that has been approved by the U.S. Food and Drug Administration (FDA) for more than 20 years to temporarily correct refractive error2; it is also an effective and enjoyable way to offer myopia control to children. This unique modality offers patients a nonsurgical opportunity for daytime spectacle and contact lens-free corrected vision, which is a freedom that can be very appealing.
In particular, children benefit from overnight wear; they are often very active in athletics and other activities that can be hindered by daily lens wear irritations, and parents appreciate keeping the lenses and lens care necessities safe at home. Getting more practitioners onboard with both ortho-k and myopia control will grow this modality and allow more patients to take advantage of these benefits.
Extensive research has been performed to attempt to show the efficacy of ortho-k in controlling myopic progression. High-level evidence, including multiple systematic reviews and meta-analysis of randomized and non-randomized clinical trials, has confirmed that ortho-k is effective in slowing axial length growth.3-6
The fitting practitioner can confidently recommend this modality, but must emphasize that both known and unknown factors may affect the degree of myopia control individual patients will achieve. It should also be emphasized that myopia control interventions cannot “undo” any myopic progression that has already occurred, and that the successes achieved by patients (and siblings) may vary widely.
IS IT SAFE?
Safety is a primary concern for any practitioner and a valid concern for patients and parents, as well. A transparent discussion outlining potential complications ranging from relatively minor and treatable (e.g., corneal abrasions, staining, lens binding, infiltrates, and/or solutions sensitivities) to major and sight-threatening (e.g., microbial keratitis) needs to occur prior to beginning any ortho-k fit.7
Overnight wear of contact lenses is associated with an increased risk of microbial keratitis,7-9 and ortho-k has been found to align with other modalities in this risk profile or to be possibly even less risky compared to overnight wear of soft lenses.2 The most common organisms implicated in severe ortho-k-related microbial keratitis are Pseudomonas and Acanthamoeba, both of which often present a serious threat to vision.8
A retrospective study of microbial keratitis in overnight ortho-k lens wear published in 2013 found that the estimated incidence was 13.9 cases per 10,000 years of patient wear in children and 0 cases in adults.9 Sharing this statistic is an easy way to convey the safety of ortho-k to parents, although it should not be used to invalidate the risk of this threat and must be accompanied by a discussion of risk factors that increase the odds of infection.
In one review, a large percentage (69%) of reported cases of microbial keratitis with ortho-k wear were determined to be from a relatively small geographical area and a brief period of time during which regulation of ortho-k lens wear and care was inadequate; due to an unusually high percentage of Acanthamoeba-related cases (33%), it was suspected that these cases were linked to the use of tap water.9 The modifiable risk factor of tap water use was again implicated in a review of Acanthamoeba keratitis cases in GP lens wearers in the United States.10
Due to the potentially serious complications of microbial keratitis (and lifelong implications in children), even if rare, ortho-k patients need to be thoroughly educated about this risk and the importance of stringent adherence to lens care recommendations. These recommendations should include proper hand-washing, avoidance of tap water contamination, no reuse or “topping off” of solution, attention to lens rubbing/rinsing and case cleaning and replacement, and compliance with any recommended follow-up appointments.
MAXIMIZING THE FIT
Today’s advanced ortho-k lens designs make it possible to effectively correct refractive error and provide good daytime vision. If myopia control is desired as well, the fitting process can now be adjusted to maximize the benefit. It is theorized that pupil size can impact the amount of myopia control that is achievable.11,12
Patients who have larger-than-average pupils have been shown to have slower axial length growth when undergoing ortho-k treatment than do patients who have smaller pupils in the same lens modality.11 In this same study by Chen and colleagues, patients wearing single-vision spectacles showed similar rates of myopic progression among groups who had different pupil sizes. This supports the theory that the peripheral defocus created by ortho-k’s steepened ring of corneal tissue outside the treatment zone is the mechanism behind this modality’s myopia control, as an eye that has a larger pupil will see more of this ring of power.11-13
While a practitioner is unable to change a patient’s pupil size with ortho-k alone, many designs now offer the option to adjust the size of the treatment zone of the lens. A smaller treatment zone could move the mid-peripheral ring of steepening closer within the pupil, resulting in more effective myopia control.10 If a patient has a larger-than-average pupil size to begin with, no changes in treatment zone are necessary; rather, keeping an average treatment zone size will help avoid unwanted visual “flare” and “glare” in dim lighting. It is for this reason that adults desiring ortho-k should always be fit with the largest treatment zone possible.
However, if a young patient has average or smaller-than-average pupil sizes and desires myopia control, a smaller treatment zone may be desirable. Additionally, young patients who have higher levels of myopia or those with more rapid progression may be better fitted in a smaller treatment zone to try to increase the retardation of their myopia regardless of pupil size, assuming they are willing to accept the possibility of some visual compromise.
Manipulating the treatment zone is relatively straightforward in most designs; the practitioner can order the initial ortho-k lenses empirically with a preferred zone size (usually between 5mm and 6mm in 0.5mm or 1.0mm steps). This parameter can also be changed throughout the fitting period or even later in the future if undesirable visual symptoms arise in a small zone or if myopic progression is greater than expected with a larger zone.14
Generally, if the fit of the lens is otherwise good, no other parameter changes need to be made if only a change in treatment zone size is desired. It is important to remember, however, that this is only the case if other fitting characteristics are suitable. Poor vision may be due to reasons other than treatment zone size. It can result from corneal staining/ocular surface issues; treatment zones that are incomplete, decentered, too shallow, too deep, or distorted by residual cylinder; or from other issues due to a poorly fitting lens.
While the practitioner does not need to make preemptive fit adjustments prior to a treatment zone size change, doing so will subsequently alter the size of peripheral fitting curves and may cause fit changes that will need to be addressed after the fact. A larger treatment zone will require one or more of the peripheral fitting curves to be made smaller (and vice versa), which can result in changes in lens stability or centration.
Monitoring corneal topographical changes is critical to success in ortho-k, but particularly when the goal is myopia control. Ultimately, the pupil and/or treatment zone sizes may be less consequential if the topographically measured mid-peripheral ring of the steepened cornea is “weak” or incomplete. This usually accompanies a generally unacceptable fit, as the central treatment, and therefore vision, is likely to be insufficient as well. This “red” ring of steepened tissue needs to be well established to induce significant peripheral retinal blur. One can estimate the dioptric change from the central flattened treatment zone to the mid-peripheral red ring of steepening via topography, and possibly infer whether the relative amount of peripheral blur induced in each patient is significant.
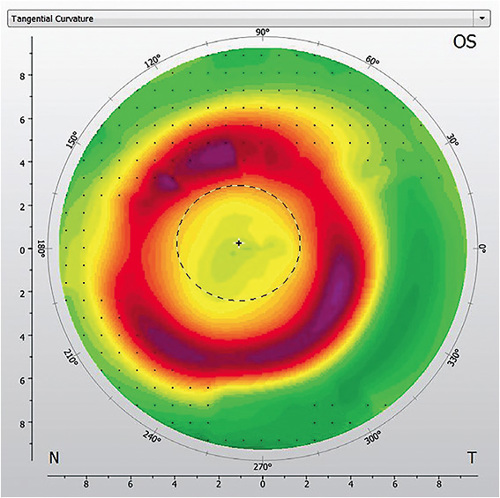
Although similar myopic control has been achieved using multiple different ortho-k lens designs,15,16 other work has shown that notably different corneal shape properties in the central and mid-peripheral zones are induced by different lens brands, particularly between four- and five-curve designs.17 In Figure 1, the central corneal curvature in this small treatment zone averages approximately 38.00D; at the steepest point in the mid-periphery, it reaches around 46.00D. This 8.00D difference is likely to be sufficient to create the peripheral blur desired for myopia control.
MONITORING MYOPIC PROGRESSION
While using instrumentation to measure axial length is the most accurate method of monitoring myopic progression in ortho-k wearers, it is not absolutely necessary for the practitioner to have to attempt in ortho-k myopia management. In fact, overzealous measurement of axial length can lead to premature attempts at treatment zone changes and/or discontinuation of ortho-k due to incorrectly perceived “failure” of the modality to effectively slow axial growth.
Myopia control is a long-term effort over many years, and decisions based on measurements made over relatively brief time frames can be premature. What looks like excessive axial length growth over six months may not actually be significant when averaged with 18 additional months of measurements.
Furthermore, in the youngest of progressive myopes (particularly those under nine years of age), myopia progression can be far more rapid than in older children.18 Ortho-k performed in younger patients may not show as much axial length growth limitation as in older children, but that doesn’t mean it wasn’t successful, and it shouldn’t be abandoned for a different treatment if the patient is doing well otherwise and the fit is sufficient. Rather, if more aggressive treatment is desired, changes in the ortho-k design or combination therapy may be a better next step than discontinuation.
If axial length measurement is not possible, the practitioner will need to monitor changes in refractive error to assess myopia control success, which can be difficult with year-to-year manifest refractions due to fluctuations based on lens wear and warpage. A reasonably reliable method of accomplishing this is to record and compare the over-refraction while the patients are wearing their ortho-k lenses after confirming that the lenses are either not warped/in good condition or newly replaced each year.
Alternatively, simply tracking any needed changes in the lens base curve radii can indicate whether or not myopic progression is occurring year to year. Retrospectively, after many years of fitting ortho-k, it can be interesting to see clinically how few patients require flatter base curve adjustments (which are made to increase myopia treatment due to progression) even after many years of wear.
ORTHO-K ADVANTAGES
Compared to other myopia control modalities, ortho-k has a few added benefits. Freedom from daytime contact lens wear is likely the greatest benefit, although there are numerous others. When compared to single-vision silicone hydrogel soft lenses or soft lens multifocals for myopia control, ortho-k can offer easier parental control of lens wear at home, participation in sports (especially water sports), fewer symptoms of dry eye,19 and potentially less damage to conjunctival goblet cell density.20
Unlike low-dose atropine, ortho-k has no potential pharmaceutical side effects. Potential ocular or systemic health risks of long-term use of low-dose atropine are still largely unknown. Therefore, it may be best to limit treatment with low-dose atropine to no longer than two years and follow it with a tapering process.21
The possibility of rebound axial growth after discontinuing any myopia control method is well known and possibly stronger during years of rapid growth and with higher concentrations of atropine.22,23 Ortho-k has no such length of use limitation and can extend well into adulthood, if desired by both practitioner and patient, and may have less potential for rebound than has been previously reported in atropine studies.9
UNIQUE PATIENT CANDIDATES
Ortho-k also offers some “outside the box” patient candidates for myopia control. Myopic children who have astigmatism can often be treated successfully with ortho-k. In 2013, the TO-SEE study reported 52% slower axial growth in children wearing toric ortho-k lenses than in control patients who had spectacle-corrected astigmatism (all with-the-rule, ranging between –1.25D to –3.50D of cylinder).24 Mild additional overcorrection can be planned for to achieve an acceptable spherical equivalent of refractive error if full astigmatic correction is not achieved by the fit alone. This may be a useful tool for patients who have against-the-rule or oblique astigmatism, as it is more difficult to achieve the lens centration and stability needed to fully eliminate corneal cylinder with ortho-k in these conditions.
For now, most ortho-k designs in the U.S. use toric peripheral curves to improve centration and to create more full and stable treatment zones in astigmatic patients; true toric base curve designs are not routinely employed and would likely be necessary to address moderate-to-high levels of astigmatism and that which is not with-the-rule. The novice ortho-k fitter is wise to address only levels of with-the-rule astigmatism lower than –1.50D until they are more experienced, as higher and different types of astigmatism present more of a challenge in fitting (specifically in lens centration).25
Interestingly, it has been proposed that the horizontal meridian of the retina (particularly temporally) is more important than the vertical meridian in driving myopic progression.26 Perhaps it is worth future study to determine if asymmetrical/toric peripheral retinal blur could be employed to exploit this, and if/how it could be accomplished via ortho-k. While it may be counterintuitive to fit off-center intentionally, it has been shown that ortho-k treatment zone decentration may further limit myopic progression so long as the patient’s uncorrected vision remains acceptable.27
Case Example: A 10-year-old healthy Asian American male was referred for possible myopia control therapy. He was an active and competitive swimmer and was very interested in contact lens wear, stating his prescription swim goggles were very blurry and inconvenient.
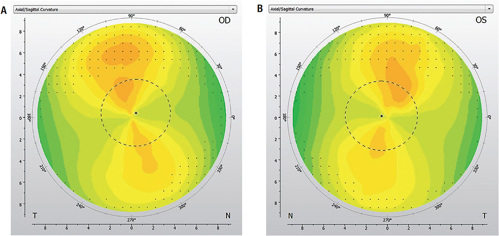
Preliminary assessment revealed spectacle refraction of –3.25 –1.50 x 013 (20/20) OD, and –3.25 –1.75 x 173 (20/20) OS. Topographies revealed regular, with-the-rule astigmatism OD and OS (Figures 2a and 2b). Anterior and posterior segment findings were unremarkable. Despite the moderate amount of astigmatism present, the patient was highly motivated to try contact lenses and his parents were interested in myopia control, so ortho-k was recommended to address both of these concerns.
A four-curve ortho-k design was ordered empirically with toric peripheral curves in the following parameters:
OD: BC 8.6mm, then peripheral curve radii of: 7.8/7.56mm, 9.2/8.87mm, and 12.0/12.0mm
OS: BC 8.6mm, then peripheral curve radii of: 7.8/7.56mm, 9.2/8.87mm, and 12.5/12.5mm
For both eyes: OAD 10.60mm, power +1.50D and OZD 6.0mm
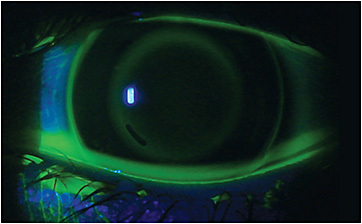
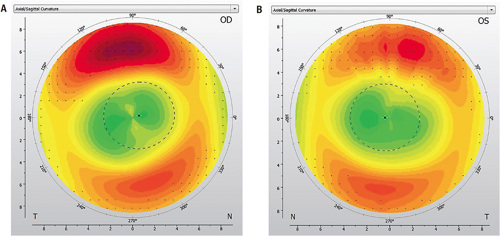
Upon dispensing, both lenses showed excellent centration and movement, with good treatment zone “bull’s-eye” patterns and acceptable edge lift (Figure 3). The patient was educated on application, removal, and care, and returned to the office for one-day and one-week follow-ups. After a few weeks of wear, uncorrected visual acuity was 20/20-1 OD and 20/20 OS, with manifest refraction of +0.25 –1.00 x 008 OD, +0.50 –1.25 x 002 OS. On follow-up topographies (Figures 4a and 4b), the treatment zones appeared well-centered OD and OS, although some residual corneal cylinder was present. Despite this, the patient was delighted with his uncorrected vision, reporting he could swim with regular goggles and see well at school all day.
While ortho-k is FDA-approved for up to –5.00D or –6.00D of myopia (depending on design), even higher amounts of myopia may benefit from at least partial treatment.28,29 The 2013 HM-PRO study found a 63% slower rate of axial elongation in children with partial reduction of myopia ortho-k compared to a control group of spectacle wearers.20 Ortho-k correction of higher levels of myopia can result in a smaller treatment zone size due to the larger amount of corneal tissue that needs to migrate from the center out to the mid-peripheral secondary zone with more significant central flattening.30 This may be beneficial for myopia control as long as vision is acceptable.
If there is an unacceptable amount of blur or visual distortion/glare, less flattening (and therefore only partial treatment) may still be useful for some myopic retardation, although the patient will be more reliant on spectacle correction during the day. Additionally, the practitioner must be wary of potentially more corneal staining with higher amounts of myopic correction.29
Another intriguing use of ortho-k is in the unilateral and/or anisometropic progressive myope. Meta-analysis of multiple studies suggests that ortho-k not only effectively slows axial growth in these patients, but can also reduce the overall total anisometropia over time.31,32 Contact lens treatment of anisometropia is often recommended to reduce spectacle-induced aniseikonia symptoms, and in monocularly myopic patients ortho-k can be performed without the asymmetrical awareness of wearing a single lens in only one eye during the day.
COMBINATION THERAPY
When discussing myopia control options with patients and their parents, the question of combining multiple therapies often arises. In particular, practitioners and astute parents may wonder if therapies that offer potentially different mechanisms of action could offer greater myopia control effect when employed simultaneously than when performed alone.
Combined use of ortho-k with low-dose atropine may be very useful in myopia control. Meta-analysis of studies comparing axial growth in patients using ortho-k alone to those using both ortho-k and low-dose atropine show that combination therapy has greater effect in slowing myopic progression than ortho-k alone.33,34 In one large analysis by Tsai and colleagues, the order of potency of axial length growth retardation was found to be highest with ortho-k combined with 0.01% atropine, then high-dose atropine (0.5% to 1%), moderate-dose atropine (0.1% to 0.25%), then ortho-k alone and low-dose (0.01%) atropine.35
While all modalities appear to show promise for myopia control, combination therapy with low-dose atropine may be the most balanced approach, considering effectiveness and potential side effects. Mild increases to this low dose of atropine (e.g., to 0.05%) may be acceptable without significantly increasing side effects.36 Additionally, if mild pupil enlargement is visually acceptable per the patient, it may further increase the efficacy of the ortho-k by allowing more peripheral distortion.
BARRIERS TO ORTHO-K
Limitations to widespread implementation of ortho-k for myopia control are numerous. There is a learning curve for practitioners interested in fitting this modality, and costs for both implementation and instrumentation can be significant. Likewise, the initial fitting cost for patients may be higher than those of other contact lens and myopia control modalities. Furthermore, as public awareness of both the need for and availability of myopia control, and even the existence of ortho-k is still relatively low, convincing parents of the need for this service can be time-consuming.
However, educational resources for practitioners are now widely available online and in person, including webinars, workshops, conferences, and numerous print material options. A positive impact on a child’s present and future refractive state can be made regardless of the boldness of the myopia control efforts. The practitioner can also add additional myopia control interventions as they become more comfortable with ortho-k fitting (Table 1).
CONSERVATIVE MYOPIA CONTROL ORTHOKERATOLOGY
|
CUTTING-EDGE MYOPIA CONTROL ORTHOKERATOLOGY
|
There is much available support from most GP lens laboratories in this endeavor, including lens design education, fitting assistance, marketing materials, and more. Having brochures, handouts, or other patient materials can reduce in-office discussion time, as can having well-trained staff to handle patient and parent questions. When cost is a concern, it is important to emphasize that the value of the practitioner’s expertise and time required for ortho-k fitting and myopia control monitoring is worth the fitting and lens fees. In addition, costs drop significantly in later years, often below those of annual supplies of other lens modalities.
CONCLUSION
When examining a patient for potential ortho-k myopia control, it is important to be mindful of more than just their refraction and keratometry measurements. The practitioner must consider their age, speed of current myopic progression, pupil size (for treatment zone considerations), visual treatment goals, personality, and level of familial support prior to recommending this modality.
Careful discussion of lens care and compliance is necessary to avoid serious complications. If patients and their parents are educated about the benefits of both ortho-k and myopia control, they are often willing to consider this modality.
The research in ortho-k and myopia control is strong and continues to grow. With greater practitioner and public acceptance, more children can be treated appropriately to limit the effects of this pandemic on their future ocular health. CLS
REFERENCES
- Holden BA, Fricke TR, Wilson DA, et al. Global Prevalence of Myopia and High Myopia and Temporal Trends from 2000 through 2050. Ophthalmology 2016 May;123(5):1036-1042.
- Bullimore MA, Johnson LA. Overnight Orthokeratology. Cont Lens Anterior Eye. 2020 Aug;43:322-332.
- Sun Y, Xu F, Zhang T, et al. Orthokeratology to control myopia progression: a meta-analysis. PLoS One. 2015 Apr 9;10:e0124535.
- Wen D, Huang J, Chen H, et al. Efficacy and Acceptability of Orthokeratology for Slowing Myopic Progression in Children: A Systematic Review and Meta-Analysis. J Ophthalmol. 2015;2015:360806.
- Si JK, Tang K, Bi HS, Guo DD, Guo JG, Wang XR. Orthokeratology for myopia control: a meta-analysis. Optom Vis Sci. 2015 Mar;92:252-257.
- Li SM, Kang MT, Wu SS, et al. Efficacy, Safety and Acceptability of Orthokeratology on Slowing Axial Elongation in Myopic Children by Meta-Analysis. Curr Eye Res. 2016 May;41:600-608.
- Liu YM, Xie P. The Safety of Orthokeratology--A Systematic Review. Eye Contact Lens. 2016 Jan;42:35-42.
- Kam KW, Yung W, Li GKH, Chen LJ, Young AL. Infectious keratitis and orthokeratology lens use: a systematic review. Infection. 2017 Dec;45:727-735.
- Watt KG, Swarbrick HA. Trends in microbial keratitis associated with orthokeratology. Eye Contact Lens. 2007 Nov;33:373-377; discussion 382.
- Cope JR, Collier SA, Schein OD, et al. Acanthamoeba Keratitis among Rigid Gas Permeable Contact Lens Wearers in the United States, 2005 through 2011. Ophthalmology. 2016 Jul;123:1435-1441.
- Chen Z, Niu L, Xue F, et al. Impact of pupil diameter on axial growth in orthokeratology. Optom Vis Sci. 2012 Nov;89:1636-1640.
- Faria-Ribeiro M, Navarro R, González-Méijome JM. Effect of Pupil Size on Wavefront Refraction during Orthokeratology. Optom Vis Sci. 2016 Nov;93:1399-1408.
- Kim J, Lim DH, Han SH, Chung TY. Predictive factors associated with axial length growth and myopia progression in orthokeratology. PLoS One. 2019 Jun 12;14:e0218140.
- Guo B, Cheung SW, Kojima R, Cho P. One-year results of the Variation of Orthokeratology Lens Treatment Zone (VOLTZ) Study: a prospective randomised clinical trial. Ophthalmic Physiol Opt. 2021 Jul;41:702-714.
- Chen R, Yu J, Lipson M, et al. Comparison of four different orthokeratology lenses in controlling myopia progression. Cont Lens Anterior Eye. 2020 Feb;43:78-83.
- Kang P, Swarbrick H. The Influence of Different OK Lens Designs on Peripheral Refraction. Optom Vis Sci. 2016 Sep;93:1112-1119.
- Marcotte-Collard R, Simard P, Michaud L. Analysis of Two Orthokeratology Lens Designs and Comparison of Their Optical Effects on the Cornea. Eye Contact Lens. 2018 Sep;44:322-329.
- Cho P, Cheung SW. Protective Role of Orthokeratology in Reducing Risk of Rapid Axial Elongation: A Reanalysis of Data from the ROMIO and TO-SEE Studies. Invest Ophthalmol Vis Sci. 2017 Mar 1;58:1411-1416.
- García-Porta N, Rico-Del-Viejo L, Martin-Gil A, Carracedo G, Pintor J, González-Méijome JM. Differences in Dry Eye Questionnaire Symptoms in Two Different Modalities of Contact Lens Wear: Silicone-Hydrogel in Daily Wear Basis and Overnight Orthokeratology. Biomed Res Int. 2016;2016:1242845.
- Carracedo G, Martin-Gil A, Fonseca B, Pintor J. Effect of overnight orthokeratology on conjunctival goblet cells. Cont Lens Anterior Eye. 2016 Aug;39:266-269.
- World Health Organization. The Impact of Myopia and High Myopia: Reports of the Joint World Health Organization-Brien Holden Vision Institute Global Scientific Meeting on Myopia. 2015 Mar. Available at myopiainstitute.org/wp-content/uploads/2020/10/Myopia_report_020517.pdf . Accessed Oct. 28, 2022.
- Tong L, Huang XL, Koh AL, Zhang X, Tan DT, Chua WH. Atropine for the treatment of childhood myopia: effect on myopia progression after cessation of atropine. Ophthalmology. 2009 Mar;116:572–579.
- Chia A, Chua WH, Wen L, Fong A, Goon YY, Tan D. Atropine for the treatment of childhood myopia: changes after stopping atropine 0.01, 0.1 and 0.5%. Am J Ophthalmol. 2014 Feb;157:451-457.
- Chen C, Cheung SW, Cho P. Myopia control using toric orthokeratology (TO-SEE study). Invest Ophthalmol Vis Sci. 2013 Oct 3;54:6510-6517.
- Maseedupally VK, Gifford P, Lum E, et al. Treatment Zone Decentration During Orthokeratology on Eyes with Corneal Toricity. Optom Vis Sci. 2016 Sep;93:1101-1111.
- Kuo HY, Hsiao JC, Chen JJ, Lee CH, Chuang CC, Sun HY. The Correlations between Horizontal and Vertical Peripheral Refractions and Human Eye Shape Using Magnetic Resonance Imaging in Highly Myopic Eyes. Healthcare (Basel). 2021 Jul 30;9:966.
- B Wang A, Yang C. Influence of Overnight Orthokeratology Lens Treatment Zone Decentration on Myopia Progression. J Ophthalmol. 2019 Nov 15;2019:2596953.
- Charm J, Cho P. High myopia-partial reduction ortho-k: a 2-year randomized study. Optom Vis Sci. 2013 Jun;90:530-539.
- Lyu T, Wang L, Zhou L, Qin J, Ma H, Shi M. Regimen Study of High Myopia-Partial Reduction Orthokeratology. Eye Contact Lens. 2020 May;46:141-146.
- Kim WK, Kim BJ, Ryu IH, Kim JK, Kim SW. Corneal epithelial and stromal thickness changes in myopic orthokeratology and their relationship with refractive change. PLoS One. 2018 Sep 25;13:e0203652.
- Tsai HR, Wang JH, Chiu CJ. Effect of orthokeratology on anisometropia control: A meta-analysis. J Formos Med Assoc. 2021 Dec;120:2120-2127.
- Zhang KY, Lyu HB, Yang JR, Qiu WQ. Efficacy of long-term orthokeratology treatment in children with anisometropic myopia. Int J Ophthalmol. 2022 Jan 18;15:113-118.
- Zheng NN, Tan KW. The synergistic efficacy and safety of combined low-concentration atropine and orthokeratology for slowing the progression of myopia: A meta-analysis. Ophthalmic Physiol Opt. 2022 Nov;42:1214-1226.
- Gao C, Wan S, Zhang Y, Han J. The Efficacy of Atropine Combined With Orthokeratology in Slowing Axial Elongation of Myopia Children: A Meta-Analysis. Eye Contact Lens. 2021 Feb 1;47:98-103.
- Tsai HR, Wang JH, Huang HK, Chen TL, Chen PW, Chiu CJ. Efficacy of atropine, orthokeratology, and combined atropine with orthokeratology for childhood myopia: A systematic review and network meta-analysis. J Formos Med Assoc. 2022 Dec;121:2490-2500.
- Yam JC, Jiang Y, Tang SM, et al. Low-Concentration Atropine for Myopia Progression (LAMP) Study: A Randomized, Double-Blinded, Placebo-Controlled Trial of 0.05%, 0.025%, and 0.01% Atropine Eye Drops in Myopia Control. Ophthalmology. 2019 Jan;126:113-124.



