
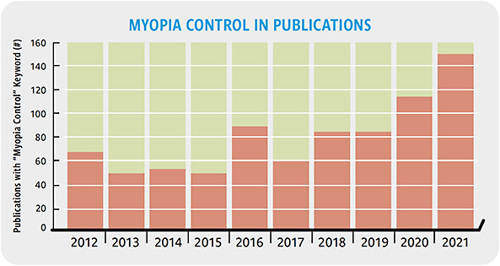
Each year, Contact Lens Spectrum provides a summary of a few key publications related to myopia control to help keep readers informed, so that they can provide optimal care for their patients. This year, I’ll present information on novel treatments for myopia control that are not yet available in the United States, the utility of past myopia progression to predict future myopia progression, low-concentration atropine to delay myopia onset and slow myopia progression, expectations related to adverse events experienced by pediatric contact lens wearers, the predictive value of choroidal thickness, and combination therapies for myopia control.
NOVEL SPECTACLES FOR MYOPIA CONTROL
Spectacle lenses that have 1.1mm highly aspheric lenslets arranged in 11 concentric rings and designed to provide myopic defocus to the entire retina slowed myopia progression 0.80D and eye growth by 0.35mm over a two-year period compared to single-vision spectacle lenses.1 This design is similar to another product not yet available in the U.S., but the lenslets in the other spectacle lenses are not aspheric or arranged in concentric rings.
Another spectacle lens was found to slow myopia progression by 0.40D and eye growth by 0.15mm over a one-year period.2 This lens is designed to reduce contrast presented to the peripheral retina, which reportedly acts as a signal to slow eye growth. Interestingly, the highest reduction in contrast did not slow eye growth as well as the lenses that provided a moderate reduction in contrast for unknown reasons.
Neither of these spectacle lenses are available in the U.S., although at least one of them may be approved for myopia control by the U.S. Food and Drug Administration as early as first quarter 2023. Hopefully, another effective myopia control modality will be available to practitioners in the U.S. in the near future.
RED LIGHT THERAPY FOR MYOPIA CONTROL
Just two three-minute periods of red light, separated by at least four hours, have been shown to reduce myopia progression and eye growth.3,4 A randomized clinical trial compared children undergoing treatment with 0.29mW of 650nm wavelength light to no treatment and found that the light therapy slowed myopia progression by 0.59D and eye growth by 0.25mm over one year.
A retrospective study showed that children undergoing light therapy with 0.40mW of 635nm wavelength light exhibited a decrease in myopia of 0.22D and eye length by 0.01mm over nine months, compared to an increase in myopia of 0.56D and eye length by 0.27mm over the same time period for patients not undergoing light therapy. While this therapy is relatively easy to administer just by having a child stare at a red light two times each day, the long-term effects on retinal integrity are unknown and the therapy is not yet available in the U.S.
PREDICTING FUTURE PROGRESSION WITH PAST PROGRESSION
Many optometrists only offer myopia control to young patients whose myopia has progressed during the previous year. However, a recent investigation showed that neither future myopia progression nor eye growth can be predicted by previous myopia progression or eye growth.5 While there was a statistically significant relationship between myopia progression over the previous year and myopia progression over the following year, myopia progression over the previous year only explained 1.3% of the variability in myopia progression over the next year. There was no relationship between eye growth over the previous year and eye growth over the next year.
While age, ethnicity, and greater baseline myopia predicted future progression, near work, time outdoors, and parental myopia did not. This indicates that eyecare practitioners should discuss myopia control with parents of young myopic children, as we cannot accurately identify the children who are most likely to progress over the next year.
LOW-CONCENTRATION ATROPINE TO DELAY MYOPIA ONSET
A retrospective study published in 2010 indicated the potential of 0.025% atropine to delay the onset of myopia.6 However, the practice of administering low-concentration atropine to pre-myopic children never really gained traction until authors indicated that—for every year later the onset of myopia occurs—an adult is expected to have –0.86D less myopia and is 2.86 times less likely to be a high myope.7
In the first randomized clinical trial to investigate the effects of 0.01% atropine in pre-myopic children, pre-myopic children were defined as 4- to 12-year-old children whose refractive error changed by more than 0.50D per year for two years and whose spherical equivalent was less than +1.00D, which doesn’t actually rule out myopic children.8 Nonetheless, results indicated a one-year change in refractive error of –0.31D for the atropine group and –0.76D for the control group. Eye growth was 0.21mm for the atropine group and 0.48mm for the control group over one year.
Several studies are underway to investigate the role of low-concentration atropine in delaying the onset of myopia, which could increase the potential of myopia control because it affects children prior to myopia onset, when eye growth and refractive error change are fastest, and it maximizes the time under myopia control treatment because it initiates myopia control immediately.
ADVERSE EVENTS OF PEDIATRIC CONTACT LENS WEARERS
As myopia control becomes the standard of care for myopic children, more are being fit with contact lenses. A report of the non-ocular and ocular adverse events experienced by 7- to 11-year-old children over a three-year period sheds some light related to expectations for pediatric contact lens wear.9 There were 432 adverse events, of which three-quarters were ocular and one-quarter were non-ocular. Contact lenses were probably or definitely related to the adverse event in almost 61% of the ocular adverse events, but only nearly 3% of the non-ocular adverse events. None of the ocular adverse events resulted in the loss of two or more lines of best-corrected vision, incapacitating or sight-threatening episodes, or permanent discontinuation of contact lenses.
The incidence of corneal infiltrative events was 185 cases per 10,000 patient-years of wear, and the incidence of ocular adverse events that required a prescription medication and was probably or definitely associated with contact lens wear was 405 cases per 10,000 patient-years of wear. Overall, adverse events experienced by 7- to 11-year-old myopic children over a three-year period rarely required meaningful treatment and never led to permanent discontinuation of contact lens wear or loss of best-corrected vision.

PREDICTIVE VALUE OF CHOROIDAL THICKNESS
Clinicians seek a parameter that predicts myopia progression in order to apply myopia control only to those who require it. A recent study of young adult myopes concluded that “choroidal thickness may be predictive of refractive error development and/or myopia progression.”10 For every 10μm increase in baseline choroidal thickness, the refractive error change was 0.006D/year less and the axial elongation was 0.003mm/year slower.
Given that the choroidal thickness changed, on average, only 10.4μm from age 20 to 28 years, the predictive value is of limited use for individuals due to the small change and high variability. The predicted changes are also so small that the clinical meaning is of little value. Therefore, choroidal changes may provide estimates of change for large samples, but they cannot be used to predict clinically meaningful changes in myopia progression or eye growth for individuals.
REBOUND EFFECT WITH LOW-CONCENTRATION ATROPINE
Children were randomly assigned to use 0.01%, 0.025%, or 0.05% atropine for two years, then individual participants in each treatment group were randomly assigned to continue with the same concentration of atropine or to discontinue treatment for an additional year. Over three years, eye growth was significantly different between the three groups, with 0.05% atropine providing the slowest eye growth (Figure 2). The 0.05% concentration also provided the highest rebound, and the difference in eye growth between those treated and those untreated over one year was 0.16mm (approximately 0.40D).
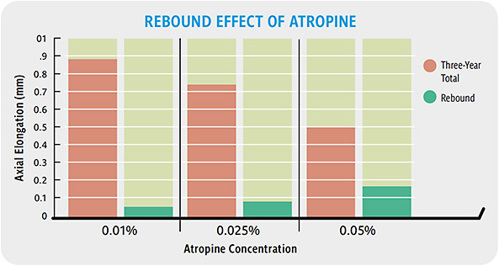
For every year older children are when they discontinue, the rebound effect is expected to be 0.05mm less eye growth. This indicates that children should maintain treatment for as long as possible to minimize the potential for the rebound effect after discontinuation. However, this does not provide any evidence that reducing the concentration of the drop prior to discontinuation will reduce the rebound effect.
COMBINATION THERAPY WITH SOFT MULTIFOCAL CONTACT LENSES AND ATROPINE
A combination of orthokeratology and low-concentration atropine provides better myopia control than orthokeratology alone,11,12 and atropine can be used as an additive therapy to slow eye growth if the practitioner or parent is not comfortable with the myopia control effects of orthokeratology alone.13 However, no other optical treatment has been examined in combination with low-concentration atropine until now.
Investigators compared myopia progression and eye growth between participants using multifocal lenses with a +2.50D add in combination with nightly administration of 0.01% atropine to historical control groups of participants using only multifocal lenses that have a +2.50D add and participants using only single-vision contact lenses.14 While both the combination therapy and multifocal lenses that have a +2.50D add alone slowed myopia progression and eye growth compared to single-vision contact lenses, there was not a statistically significant or clinically meaningful difference between the combination therapy and contact lens therapy alone. The investigators did not have a good explanation of why combination therapy may be more effective than monotherapy for orthokeratology but not soft multifocal contact lenses alone.
SUMMARY
The research highlighted in the 2022 update on myopia control is not comprehensive of the myopia control literature, but it points out some of the important clinical issues that face clinicians when treating young myopes. With the growing body of evidence that several forms of myopia control are effective, it is beginning to replace simple alleviation of distance blur as the standard of care for young myopic patients.
Given this increasing body of myopia control evidence, eyecare practitioners must critically evaluate the literature to watch for emerging trends and provide evidence-based medical care. With new treatments on the horizon, eyecare practitioners should learn about novel treatments that may not yet be available in the U.S., such as myopia control-specific spectacles and alternative therapies that may slow eye growth and ultimately reduce risks.
Likewise, practitioners must base management plans on scientific evidence, which indicates that knowing the prior progression of a myopic child does not mean that the patient is a better candidate for myopia control. Furthermore, no current ocular parameters are capable of predicting future myopia progression, including choroidal thickness. The small magnitude and large variability of choroidal thickness measures limit the usefulness of choroidal thickness as a predictor of future myopia progression for individuals. Instead, parents of all myopic children should receive appropriate informed consent so that they can play a role in deciding the most appropriate care for their child.
Likewise, we are not yet capable of individualized treatment for myopia control. In fact, the complicated genetics and environmental effects related to myopia progression most likely mean that we will never have individualized treatments similar to those for single-gene mutations that cause certain cancers. We do not know the treatment that will provide the best myopia control for the patient in the chair.
Therefore, if you or the parent believe that you did not achieve sufficient myopia control with the first treatment, you should add a second treatment rather than switch treatments. Several studies have indicated that combination therapy with orthokeratology and low concentration atropine provide better myopia control than monotherapy, but interestingly, combination therapy with soft multifocal contact lenses and low-concentration atropine do not provide additional benefit.
Children exhibit slower myopia progression and eye growth with 0.05% than with 0.025% or 0.01% atropine, but the higher concentration results in greater rebound after discontinuation. In order to reduce the rebound effect, therapy with low-concentration atropine should be administered as long as possible because older age at discontinuation results in less rebound.
Overall, 2022 provided much meaningful information about myopia control, ranging from delaying the onset of myopia to when to discontinue myopia control. To practice full scope optometry in an evidence-based manner, you must read the literature, attend continuing education seminars, and interact with colleagues. These actions will provide parents with confidence in you and ensure appropriate care for your patients. CLS
References
- Bao J, Huang Y, Li X, et al. Spectacle Lenses with Aspherical Lenslets for Myopia Control vs Single-Vision Spectacle Lenses. JAMA Ophthalmol. 2022 May;140:472.
- Rappon J, Chung C, Young G, et al. Control of myopia using diffusion optics spectacle lenses: 12-month results of a randomised controlled, efficacy and safety study (Cypress). Br J Ophthalmol. 2022 Sep 1;bjophthalmol-2021-321005.
- Zhou L, Xing C, Qiang W, et al. Low-intensity, long-wavelength red light slows the progression of myopia in children: an Eastern China-based cohort. Ophthalmic Physiol Opt. 2022 Mar;42:335-344.
- Jiang Y, Zhu Z, Tan X, et al. Effect of Repeated Low-Level Red-Light Therapy for Myopia Control in Children: A Multicenter Randomized Controlled Trial. Ophthalmology. 2022 May;129:509-519.
- Mutti DO, Sinnott LT, Brennan NA, Cheng X, Zadnik K; Collaborative Longitudinal Evaluation of Ethnicity and Refractive Error (CLEERE) Study Group. The Limited Value of Prior Change in Predicting Future Progression of Juvenile-onset Myopia. Optom Vis Sci. 2022 May 1;99:424-433.
- Fang PC, Chung MY, Yu HJ, Wu PC. Prevention of myopia onset with 0.025% atropine in premyopic children. J Ocul Pharmacol Ther. 2010 Aug;26:341-345.
- Chua SY, Sabanayagam C, Cheung YB, et al. Age of onset of myopia predicts risk of high myopia in later childhood in myopic Singapore children. Ophthalmic Physiol Opt. 2016 Jul;36:388-394.
- Jethani J. Efficacy of low-concentration atropine (0.01%) eye drops for prevention of axial myopic progression in premyopes. Indian J Ophthalmol. 2022 Jan;70:238-240.
- Giannoni AG, Robich M, Berntsen DA, et al. Ocular and Nonocular Adverse Events During 3 Years of Soft Contact Lens Wear in Children. Optom Vis Sci. 2022 Jun 1;99:505-512.
- Lee SS, Alonso-Caneiro D, Lingham G, et al. Choroidal Thickening During Young Adulthood and Baseline Choroidal Thickness Predicts Refractive Error Change. Invest Ophthalmol Vis Sci. 2022 May 2;63:34.
- Kinoshita N, Konno Y, Hamada N, et al. Efficacy of combined orthokeratology and 0.01% atropine solution for slowing axial elongation in children with myopia: a 2-year randomised trial. Sci Rep. 2020 Jul 29;10:12750.
- Tan Q, Ng AL, Choy BN, Cheng GP, Woo VC, Cho P. One-year results of 0.01% atropine with orthokeratology (aok) study: a randomised clinical trial. Ophthalmic Physiol Opt. 2020 Sep;40:557-566.
- Jones J, Mutti D, Jones-Jordan L, Walline J. Effect of Combining 0.01% Atropine with Soft Multifocal Contact Lenses on Myopia Progression in Children. Optom Vis Sci. 2022 May 1;99:434-442.
- Huang J, Mutti DO, Jones-Jordan LA, Walline JJ. Bifocal & Atropine in Myopia Study: Baseline Data and Methods. Optom Vis Sci. 2019 May;96:335-344.




