
GP LENSES, either corneal or scleral, are routinely prescribed to correct refractive error or irregular astigmatism for visual improvement. Typically, these lenses are prescribed for daily wear to avoid the increased risk of corneal inflammation or sight-threatening microbial keratitis. The overnight use of GP lenses for orthokeratology is an exception to this, but a recent study indicates that the benefits of reducing myopia outweigh the risks (Bullimore et al, 2021; Chiu, 2023).
Some disabled or elderly patients need GP lenses for improved functional vision but are unable to physically apply or remove lenses. These patients can benefit from extended wear corneal GP lens wear.
CASE EXAMPLE
An 86-year-old female with Fuchs’ corneal dystrophy had penetrating keratoplasty of her right eye in 2011. She had a history of previous cataract surgery and herpes simplex keratitis posttransplant surgery. Slit lamp exam showed a relatively clear right cornea with minimal scarring and vascularization. She also had significant ptosis, blepharitis, dry eye, and filamentary keratitis. Her best-corrected visual acuity (BCVA) with manifest refraction was –1.50DS 20/200.
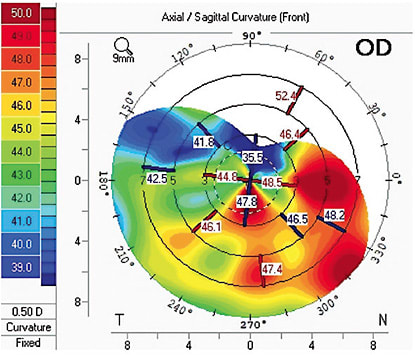
Corneal topography (Figure 1) showed severe corneal irregularity that was limiting her visual acuity with glasses correction. The patient was educated that a GP contact lens would significantly improve her visual acuity. This was especially critical because the BCVA of her left eye was 20/200 due to corneal edema secondary to Fuchs’ dystrophy, and she was reluctant to undergo transplant surgery.
It was determined that the patient, who lives alone, would be unable to successfully apply and remove a GP lens and, therefore, she was fit with a GP corneal lens to be worn on a four-week extended-wear basis. The patient’s most recent lens is an intralimbal design with a diameter of 11.5mm and a base curve of 42.87, is made of hexafocon A (off-label), and has a power of –1.00D. Her BCVA was 20/25. She instills rewetting drops two to four times per day for lubrication. She returns monthly for lens removal and cleaning, as well as monitoring for adverse events. The lens does have to be applied with a drop of artificial tears in the bowl to prevent air bubbles (Figure 2).
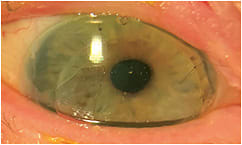
Her contact lens use has been interrupted twice due to complications. Four years prior, she experienced corneal graft rejection that resolved after four weeks of topical steroids. Later that same year, she reported with irritation secondary to sterile inflammatory keratitis, which resolved after one week of steroid treatment.
This case is an example of how much GP lenses can improve the quality of life for a patient who would otherwise be visually impaired. After discussion and education, it was agreed that the patient benefited from wearing the GP lens for extended periods despite the increased risk of inflammation and infection. Daily lubrication of the lens with supplemental artificial tears is critical to prevent lens adherence and corneal desiccation. The patient is monitored for corneal edema, vascularization, and infiltrative keratitis. CLS
References
- Bullimore MA, Ritchey ER, Shah S, Leveziel N, Bourne RRA, Flitcroft DI. The Risks and Benefits of Myopia Control. Ophthalmology. 2021 Nov;128:1561-1579.
- Chiu G. Sleeping in Lenses. Contact Lens Spectrum. 2023 June;38:18.



